| Download PDF Version |
 Dear Friends,
Dear Friends,
I am very pleased to report that Stony Brook Medicine is rising! Wonderful things are breaking out all over.
Joining our cadre of new Department Chairs, who include Vince Yang MD, PhD (Medicine), Dennis Choi MD, PhD (Neurology), Ramin Parsey MD, PhD (Psychiatry), Todd Griffin MD (Obstetrics/Gynecology), and Mark Schweitzer MD (Radiology), our new Deans, who include Lina Obeid MD (Research), Meenakshi Singh MD (Faculty Affairs) and Basil Rigas MD (Clinical Affairs), our new University Hospital CEO Rueven Pasternak MD, and our new Institute/Program Directors, who include Lisa Benz-Scott PhD (Public Health), Yusuf Hannun MD (Cancer Center), and James Taylor MD and Harold Fernandez MD (Heart Institute), are Mark Talamini MD, our new Chair of Surgery, and Joel Saltz MD, PhD, our new Chair of Biomedical Informatics. In fact, Joel’s department is also new, designed to capitalize on the (extremely) big data generated from the medical histories, physical examinations, laboratory values, radiological scans and pathology specimens of the nearly 250,000 patients seen at Stony Brook Medicine every year. Each of our departments is also expanding our faculty ranks, to bring even more research, educational and clinical expertise to our campus.
I am also pleased to report that much work is underway on our efforts to reform our medical school curriculum. Thirteen “learning communities” are forming in the Fall, composed of (note: not led by) three faculty members, ten students from each class, and the shining spirit of medicine past, derived from the legendary physician for whom each community is named (e.g. Osler, Taussig, Cushing, Koch, Addison, Lister, Blackwell, Laennec, etc.). We are also making much progress on shifting the transition from completing preclinical coursework to beginning clinical clerkships, moving June back to March of Year Two, and creating educational translational pillars for the third and fourth years, designed to consolidate the biochemical/physiological/ immunological/anatomical/pharmacological basis of clinical conditions and their resolution.
In the realm of outstanding, patient centered, compassionate clinical care, we learned that Stony Brook Medicine scored 19 “Best Doctors in New York”, an all-time high for us, and, for the second year in a row, the clinical quality of University Hospital was rated “A” by Leapfrog, one of the oldest and most extensive hospital quality evaluation websites in the United States.
And we continue to modernize our campus. Plans are on schedule for our hospital expansion and MART (Medicine and Research Translation) buildings, holding nearly 500,000 sq ft of new clinical, educational and research space, with construction scheduled to begin in October, and official ground-breaking in January. The hospital expansion will house Stony Brook Children’s Hospital, a state of the art facility to care for our most vulnerable patients, as well as new “acuity adjustable beds” and intensive care units. In July, the Cancer Center took delivery of one of the very first in the nation simultaneous PET/MRI scanners, for both experimental and clinical use, which will be used in numerous cardiac, neuropsychiatric and cancer applications. The ribbon cutting ceremony is scheduled for October. And we will create 650 new parking spaces on campus; construction will begin this summer on two surface lots on the western and southern sides of the east campus power plant. As they say, “please pardon our dust”, as the entrance to the hospital garage is re-oriented, to accommodate the two new surface lots and a new road that will connect to the new bed tower and MART building entrances.
 As we begin yet another cycle of new entering students, I am reflecting on the fact that this is my fourth year in this role at the School of Medicine. A lot has happened and is continuing to happen.
As we begin yet another cycle of new entering students, I am reflecting on the fact that this is my fourth year in this role at the School of Medicine. A lot has happened and is continuing to happen.
Looking back, three major things have happened:
Accreditation
First, as part of our LCME accreditation process, we did a real self-assessment and made significant changes to our curriculum and its administration. We have instituted systematic quality control processes and analyses to identify strengths and weaknesses pro-actively. We developed a full- fledged clinical campus at Winthrop University Hospital. Those efforts paid off and we have a fully accredited medical school. The accrediting body is not coming back until 2018. All of you will have graduated by then.
Student Feedback
Second, we decided to find out how the students were experiencing the school. We created more opportunities for them to tell us safely how things really were. Surveys, focus groups, and exit interviews are now part of our routine. And we listened. These are some of the changes that happened as a direct result of their feedback.
Some Changes Instituted
We instituted a weekly email TGIF (Timely General Information on Fridays) to enhance communication. Additionally, we do a quarterly newsletter, VIDYA, to provide students with the details of the educational changes and happenings at Stony Brook. We changed the grading system in the first two years. In the second year, we combined systems courses, reducing the number of exams and thereby the constant stress. We used customized and integrated NBME exams for all systems. We restructured the Pharmacology course to integrate within Systems. In the third year, we made sure that all students received mid clerkship feedback in all clerkships. We also allowed flexible electives, and made major changes to the fourth year. We eliminated unnecessary requirements, enhanced our Subinternships and added two new courses, Transition to Residency and Advanced Clinical Experience. In general, all of these changes have been favorably received by the student body.
Learning Environment
Third, we recognized that the learning environment of our students was not optimal. Our efforts to educate, inform and enforce our values of ICARE (Integrity, Compassion, Accountability, Respect and Excellence) resulted in the creation of the WESMILE program (We can Eliminate Student Mistreatment In the Learning Environment). We are happy to report that most recent data show that all of our students are aware of what our mistreatment policies are and how to report concerns. Our progress in this area is quite satisfying.
So What Is Going On Now?
We are changing our curriculum. Last December, the Curriculum Committee approved 14 guiding principles. The primary goal of the change is to focus on LEARNING, encouraging self-direction, integrated and active learning, as well as reflection and teamwork in medical practice. Seven subcommittees and approximately 100 faculty and students are involved in the discussions and deliberations so that we generate the best ideas for innovations in the new curriculum. The new curriculum will allow early entry into the clinical phase of training and contextual reinforcement of basic science concepts in the clinical years. The entering class of 2014 will experience the new curriculum.
Longitudinal Learning Communities: We have just started 13 learning communities in the school to provide our students with a more personalized way to connect with our faculty. Please see more on that in Dr. Fleit’s column.
Academy of Clinical and Educational Scholars (ACES)
We are just beginning to create an Academy to recognize the creativity of our outstanding educators and to enhance scholarship and visibility among our educators. We expect a fully functioning academy by AY 2014-15. Thanks to the endowment from the family of a grateful student, this is now possible at Stony Brook.
Finally, I will be tweeting periodically important events that students should know about. We heard from the students that they wanted to get important news in less than 140 characters. We will try. Follow me at #drlathachandran.

For the academic year beginning 2013, the School of Medicine is establishing a new component entitled Longitudinal Learning Communities (LLCs). These LLCs will provide a community-based approach to learning and will encourage students to interact with faculty and their peers in a safe environment. We anticipate that the LLCs will provide a venue for our students to develop skills in team-work, peer-group evaluation and feedback mechanisms to help students develop skills in a team-based collaborative approach to the practice of medicine.
Each LLC will consist of three faculty facilitators and ten students from each class who will belong to the LLC over the four years of medical school. Additionally, student-centered leadership of each of the LLCs will ensure vitality and innovation. LLCs will meet monthly and will focus on advising, mentorship, team work and peer feedback.
The small group environment of the LLC will enable informal and formal interactions between students and faculty and among students and their near peers. Among the activities planned for the LLCs are career counseling, academic schedule planning, community service or common group projects, and communications regarding key issues in medical education and health care.
The thirteen Longitudinal Learning Communities are named after noted physicians and scientists:
| Virginia Apgar | William Harvey | William Osler |
| Elizabeth Blackwell | Robert Koch | Helen Taussig |
| Harvey Cushing | Rene Laennec | Paul D. White |
| Charles Drew | Joseph Lister | |
| Sigmund Freud | Elie Metchnikoff |
The Scholarly Concentrations Program is a four-year track opportunity for medical students to engage in and attain recognition for scholarly pursuits in related areas of medicine. Under this Program, students have the opportunity to do academic exploration in Basic Sciences, Translational Research, Global Health, Medical Education, Social Science or Medical Humanities & Ethics. The program aims to align the areas of interest of students with the academic mission of the School providing a longitudinal area of work to the student experience at the School of Medicine. For many students, this period has been extremely helpful in shaping career goals and in building an academic track record attractive to residencies. The specific goals of the Scholarly Concentrations Program are:
- To provide encouragement, impetus, and support for engaging in additional extracurricular scholarly pursuits aligned with one’s own area of interest
- To facilitate the attainment of valuable career experience in areas and projects related to medicine as a complement to students’ didactic medical education.
- To provide special recognition to students who engage in such scholarly pursuits and meet the standard requirements of the program.
A Research Day is held every year in the spring to give graduating students an opportunity to present the results of their research in an oral and/or poster presentation. A research award is given to an outstanding student chosen by the SCP committee as part of the graduation festivities. You can learn more about this program online at: http://medicine.stonybrookmedicine.edu/firstyearresources/mdscholar
By Arjun Iyer and Kaveh Moghbeli
 The beginning of medical school and the symbolic donning of the white coat mark an important transition for the new medical student. While the acquisition of knowledge remains as important as it was in the undergraduate years, a new challenge emerges: the development of a new identity as a medical professional. However, whereas medical knowledge is easily standardized and assessed, measuring a student’s progress towards the ideals of the medical profession remains difficult and elusive.
The beginning of medical school and the symbolic donning of the white coat mark an important transition for the new medical student. While the acquisition of knowledge remains as important as it was in the undergraduate years, a new challenge emerges: the development of a new identity as a medical professional. However, whereas medical knowledge is easily standardized and assessed, measuring a student’s progress towards the ideals of the medical profession remains difficult and elusive.
Subgroup 3, the student-run arm of the Curriculum Evaluation Working Group (CEWG), is working towards a system of ongoing peer evaluation and self-assessment that will come into effect in the fall of 2014. Our ultimate goal is to employ three components that facilitate the continued development of professional character:
- Evaluations from Peers: Drawn from peer assessments to understand our own strengths and weaknesses and use this knowledge to build our proficiency in interpersonal communication and group responsibility.
- Evaluations of Peers: Learn to educate others in a timely yet sensitive manner.
- Self Evaluation: Develop self-awareness by comparing self evaluations to evaluations from peers. Understand that while you may not always be given feedback during your career, you have the ability to constantly self-assess and improve.
We anticipate that feedback will be delivered via CBase, and over time, students will accumulate a database that they can use to guide their development. These exercises will be purely formative (not graded) in order to encourage honest communication and intrinsic motivation to seek input. Finally, faculty and upperclassmen will go over each of these three areas with students at regular intervals to teach students how to give feedback and use the feedback they receive to improve their performance.
At this point, we are working to integrate peer feedback with the learning communities and research ways to foster student professionalism. We are currently recruiting new members from all classes, so if you would like to help direct curriculum development at one of the most dynamic points in Stony Brook history, please contact Arjun (arjun.iyer@stonybrookmedicine.edu) or Kaveh (kaveh.moghbeli@stonybrookmedicine.edu).
A new site has become available to the Ob/Gyn clerkship. In addition to Stony Brook, Winthrop, and NUMC we now have the pleasure of announcing our new site, Southampton Hospital. For the academic year, 2013-14, the Ob/Gyn clerkship will have students at this site from July to December (3 Blocks). Students can spend their summer in the Hamptons while delivering babies! Students have the chance to work one on one with attendings during their Ob/Gyn clerkship while “gallivanting” around the Hamptons in their free time. The Fall is also beautiful in the Hamptons!
This location is a community hospital with dedicated faculty who are excited to teach Stony Brook students the art of Ob/Gyn. The staff has many years of expertise and have also experienced teaching osteopathic students who were rotating through there; but with our new agreement, Southampton Hospital is excited to align themselves with Stony Brook and the opportunity to teach Stony Brook students instead. Students will be working only with attendings in their office, the public clinic, and the hospital during the entire 8 weeks of the clerkship. The site director, Dr. Alamia, is a former resident of Stony Brook with a very successful practice. The GME office is very efficient and highly capable with years of experience with rotating students.
Housing is also available. The living units are single and double bedroom apartments. The double bedroom apartments have a shared, updated kitchen, bathroom and common living area. The apartments are air conditioned, fully furnished, and have internet and cable TV access. Laundry facilities are also available. The apartments are waterfront and the view is spectacular! They are located 9 miles from the hospital.
The Hamptons is a beautiful and very popular location on the east end of Long Island with surrounding beaches, the vineyards, and the LIRR available. The Orient Point ferry is nearby as well, in case students want to get to Connecticut, Massachusetts or Rhode Island. During the summer and fall, people flock to this end of the island for the beaches and the wineries.
If you are interested in applying for the Southampton Site for your Ob/Gyn clerkship, you will be able to request it as one of the possible sites when you register for year 3 clerkships.
Students who are spending July and August in their Ob/Gyn clerkship at Southampton have provided comments about their experiencs:
“Southampton has been a cool experiment so far….everyone at SHH is warm, friendly, and welcoming as well as receptive to our suggestions as to how to improve the OB/Gyn experience for SB students. Working around DO’s offers a refreshingly comprehensive view of medicine of not only the patient, but the Hamptons community as a whole. Living on the bay 5 minutes from the ocean is also a beautiful experience!” — Michael R. Locher, MSIII
“Southampton is going pretty well. It’s a nice little community hospital with a big emphasis on community. One particular thing I’ve noticed is that people around here do not pass each other in the hallway without saying hello. The main hospital building consists of just three floors, making it easy to find your way around….
“There is plenty of opportunity to do things when it gets busy as they do not have an OB/GYN residency, so the med student assists the attending directly. My first day there I assisted with a cesarean and pulled the placenta out of the uterus….
“They have us housed in a small complex in Hampton Bays, sitting right on the water with a view of the bay and Fire Island in the background. The view is very nice during the day and at night. There is a pool too. The building is occupied by other medical students and residents and is located in Hampton Bays, about 9 miles west of the hospital. The studio I live in is pretty nice, fully furnished, and the kitchen has a full oven and fridge. It takes about 20 minutes to drive to the hospital in the morning….” — Yevheniy Lider, MSIII
National Standardized Exams.
Our students consistently perform at or above the national average.
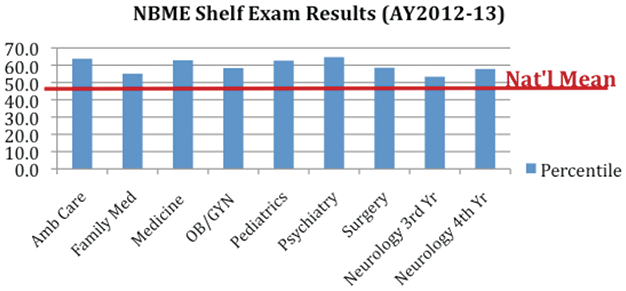
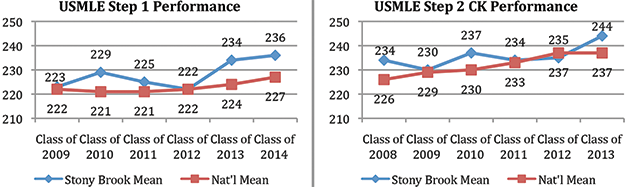
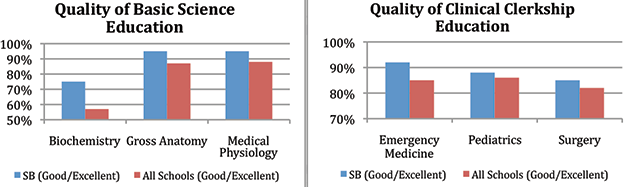
AAMC Medical School Graduation Questionaire.
Our graduates are satisfied with the quality of their medical education training.
In addition to being named a Distinguished Teaching Professor, the award that constitutes the highest system tribute for teaching conferred upon a State University of New York faculty member, Jack has received the Chancellor’s and the President’s Awards for Excellence in Teaching, been inducted into Alpha Omega Alpha, received a Citation for Excellence in Teaching by the Medical School Graduating Class 15 times, and has been selected to be a Hooding Ceremony Participant more than a dozen times. It is no accident that one of the first recipients of the Aesculapius Award for Excellence in Teaching in the School of Medicine was Jack Stern. But perhaps a comment from a former student best summarizes Professor Stern’s character as a standard-bearer for quality of instruction when he describes him as “…our Virgil through the portion of medical school best described as L’Inferno. He establishes a personal and academic standard from the first day of our experience which few faculty will rise to meet. He brings out the best in his students, and is fondly remembered as the man who gave them the first taste of the commitment, sacrifice, and reward inherent in the study of medicine.”
Directing “The Body” course is not the only leadership role Jack has played in his many years at Stony Brook. He has chaired subcommittees for LCME Self Studies, served as the Chair of the Curriculum Committee, and most importantly to me personally, was Chair of the Department of Anatomical Sciences beginning in 1990 at a critical time when the department was undergoing restructuring. Jack continued at the helm, steering us through many difficult times until 2006, when he stepped down as chair. When we were designing the brashly modified version of Rembrandt’s “The Anatomy Lesson of Dr. Tulp” for our departmental web page (reproduced here), there was no question as to who would be portrayed in the central role of the cadaver – it could only be Jack who has always “led by example.”
In addition to his teaching contributions, few faculty members in the School of Medicine are more giving of their time outside of class than Jack. Students and colleagues alike marvel at his dedication in attending graduation ceremonies, match day, and school social functions such as the annual pot-luck dinner/talent show, reunion dinners, and the Evening of the Arts. At the same time, Jack has maintained a highly productive career as a research scientist establishing a unique research laboratory for the study of primate locomotion that has been referred to by one grant reviewer as a “national treasure.”
I know there is no way I can ever fill Jack’s shoes, but I can strive to maintain the standards he has set for the delivery of “The Body” course. Having worked alongside him for more years than I like to admit, I share his commitment to providing our students the very best preparation in gross anatomy for their future careers. Fortunately for me, Jack has written down all he knows in two textbooks…..
The School of Medicine has MSTP, MD/MBA and MD/MPH programs.
These are considered to be joint degree programs during which students
complete the MD degree and either a Masters in Business, a Masters in
Public Health or a PhD degree in a research field.
For the MD/MBA, the students apply to the School of Medicine and
indicate that they are interested in the MBA program. They are accepted
to the School of Medicine first, followed by acceptance to the School of
Business. The MBA is 48 credits consisting of 16 courses. Students can
take most of the MBA before starting medical school or after completing their medical degree. Some students opt to take a year off from medical school to complete the bulk of their MBA courses. Ethics and Law, and an Industry Project offer credit in both the MD and MBA programs. [from http://www.stonybrook.edu/commcms/business/mba/md_mba.html You can find more information at this website.]
The MSTP, or Medical Scientist Training program, enables students to complete a PhD and an MD as part of a joint degree program. Students start medical school and complete the first two years, and their USMLE Step 1 licensing exam before beginning their PhD research. Students often take 3 to 5 years to complete their PhD, after which they return to the clinical years of medical school. Students have opportunities to present their work at “Research Days” at the university, or at national or regional conferences. They work with scientists at Brookhaven National Laboratory and Cold Spring Harbor Laboratory. The MSTP website states, “Graduates of this program are equipped to study major medical problems at the basic level, and at the same time, to recognize the clinical significance of their discoveries” [from http://www.pharm.stonybrook.edu/mstp/ You can find more information at this website.]
“The MD/MPH Program advocates a population health approach to public health. The hallmarks of population health are an ecological understanding of the determinants of health and a systems approach to solving health problems; emphasis on proactively stabilizing and improving health among all populations; and insistence on accountability, evidence-based practice, and continuous performance improvement” [From http://publichealth.stonybrookmedicine.edu/career. You can find more information at this website]. The program focuses on developing public health leaders who will make an impact on society. Students in the MD/MPH program can take Global Health, Epidemiology, and Biostatistics courses in the MPH program and receive elective credit weeks in the medical school.
This course was created to address previous student concerns about feeling inadequately prepared for residency training. The TTR course included a series of lectures, team-based learning sessions, small-group case discussions, procedure laboratories, high fidelity simulation cases and a series of electrocardiogram workshops. Additionally, students were recertified in Basic Life Support and Advanced Cardiac Life Support. The topics were designed to be case-based, very practical and highly interactive; and, they covered numerous useful topics including management of shock, communication across specialties, pediatric resuscitation, top 10 intern night calls and managing finances. I directed the course and my faculty spanned multiple specialties throughout our institution. I selected the finest teachers amongst us and they were praised for their enthusiasm and commitment.
Overall, students loved the course. They found the content to be right at their level and it was delivered in a highly practical fashion so that they could easily translate it towards their post graduate training. Students left the course feeling much less anxious about the year ahead of them. Together the students and my faculty came up with ways to make the course even better for this year.
|
CONGRATULATIONS to three of our first year medical students, Class of 2016, who received the McGraw-Hill Lange Award! The award was given to students who excelled in their studies during the first year and were nominated by the faculty for their outstanding performance. The students were: |
|
|
Our students are well represented on our School Committees. Feel free to talk to your committee representatives to find out what’s going on regarding policy, curriculum, and other important committees. See if you can participate and help! Committee on Academic Standing Honor Code Curriculum Committee Clinical Course Director’s Committee Student Finance Committee Pedagogy Review (CEWG) Learning Communities |
| TGIF: Read your TGIF emails from the UME office every Friday. Get news, important scheduling information, research and elective opportunities, etc. | ||
| Learning Communities: Keep your eyes open for more information coming this Fall | ||
| Student Activities in 2013-14: | ||
| First Year Orientation | August 16-23 | Noon-4pm |
| White Coat Ceremony | August 18 | Noon-4pm |
| Second Year Welcome Back | August 19 | Noon-4pm |
| International Opportunities Sessions | September 11, October 15 | Noon-4pm |
| Hispanic Heritage Event | October 18 | 6-10pm |
| Scholarly Concentrations Info Session | November 18 | Noon-1pm |
| Year 3 Intersession | December 16-20 | all day |
| Year 2 Intersession | January 2-3 | all day |
| Diaspora of Color | January 17 | 6-10pm |
| Evening of Art | Feburary 19 | 6-10pm |
| Asian Extravaganza | March 7 | 6-10pm |
| Match Day | March 21 | Noon-2pm |
| Pot Luck Dinner | April 14 | 6-10pm |
| Research Day-SCP presentations | May 7 | 8:30am-Noon |
| Commencement | May 22 | 10am-Noon |
| Year Three Orientation Week | June 23-27 | all day |
| Also check the School’s Academic Calendar at: https://cbase.som.sunysb.edu/conet/calendar/stud_mainFrame.cfm?school=Medicine |
||
A series of seminars & workshops for medical, nursing & dental students who want to communicate more effectively about health science with patients, the public, public officials, the media, etc. Directed by Evonne Kaplan-Liss, MD, MPH, with guest lecturers from Alan Alda Center for Communicating Science & SB School of Journalism. Time: 4-7PM. 10/2,9,23, 11/6,13, 20. Add with dropadd form.
Global Health is an elective taken by year 1 & 2 students, usually held from 4-5pm one day a week. Course objectives: Being able to describe the most important causes of mortality & morbidity in low-income countries; being aware of initiatives to combat health problems in the countries including vaccination programs; understanding the impact of malaria, other illnesses on public health; being able to place medical problems & interventions in cultural, socioeconomic & demographic context with emphasis on the role of women, etc. Add with drop/add form.
The Rising Leaders in Health Care elective begins in November. The core goals are: Gaining real-world, applicable skills; Enhancing professional networks; Building community relationships; Expanding cultural awareness; Evaluating healthcare industry efficiency and effectiveness; Improving the quality of patient care. Please sign up with a drop/add form if you would like to add the class for credit.
| Download PDF Version |

