 One of the greatest challenges to improving patient care is the heterogeneous mix of patients undergoing cardiac arrest as well as the heterogeneous nature of the medical and nursing staff across a multitude of disciplines who typically care for these patients. Thus, standardization of care and implementation of the latest American Heart Association guidelines (as the standard of care) is a major challenge in any institution. At our institution, improvements were achieved through enhanced training and education methods beyond standard advanced cardiac life support (ACLS)) for medical and nursing staff (Resuscitation Plus) together with the introduction of innovative resuscitation methods focusing on the quality of oxygen delivery to the brain and other vital organs.
One of the greatest challenges to improving patient care is the heterogeneous mix of patients undergoing cardiac arrest as well as the heterogeneous nature of the medical and nursing staff across a multitude of disciplines who typically care for these patients. Thus, standardization of care and implementation of the latest American Heart Association guidelines (as the standard of care) is a major challenge in any institution. At our institution, improvements were achieved through enhanced training and education methods beyond standard advanced cardiac life support (ACLS)) for medical and nursing staff (Resuscitation Plus) together with the introduction of innovative resuscitation methods focusing on the quality of oxygen delivery to the brain and other vital organs.
Our program led to a 30% increase in survival, which rose from a baseline of 21-23% during the period 2006-2010 to 33% for two years in row (2012 and 2013); earning our quality improvement program within Stony Brook University Hospital a “bronze award” from the American Heart Association for significant improvements in cardiac arrest resuscitation care in 2012. Our survival exceeded the national US in-hospital survival rate of 18-25%. Overall, 84% of patients who survived to hospital discharge achieved a favorable neurological outcome (functionally independent at discharge). A 70% increase in survival was also observed for patients undergoing cardiac arrest outside of the hospital. A gradual rise in survival rates was observed year on year from 4% in 2010, to 6% in 2011, to 9% in 2012, and 13% in 2013 1 (compared to a national average rate of 5-9%). Survival rates have persistently remained at 13-14% since 2013.
Note 1: These data were independently provided by the hospital continuous quality improvement (CQI) office as well as the emergency department and were achieved without changes to patient selection or inclusion criterion.
Reporting Cardiac Arrest and Post-Resuscitation Outcomes
A comprehensive post-resuscitation management program has also been created as well as a dedicated quality reporting dashboard relating to both intra cardiac arrest and post resuscitation (ICU) variables. The Stony Brook Post-Resuscitation dashboard was created approximately 12-24 months before a similar dashboard was introduced by the American Heart Association’s “Get With The Guidelines - Resuscitation” program, which Stony Brook remains part of.
Educational Programs
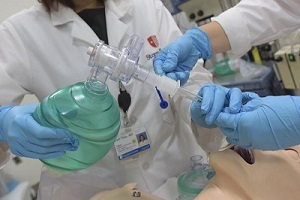
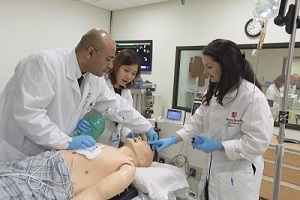
 The education component has been disseminated with the help of other key members and in particular Dr. Barbara Mills (Director of Rapid Response Service) and Dr. Sahar Ahmed (Faculty in Pulmonary & Critical Care). This has been an on-going program in which medical residents and critical care fellows receive enhanced training through a combination of didactic and simulation methods. These efforts were combined with focused lectures, meetings and discussion with hospital leadership, nursing leadership and key faculty in all the divisions and departments involved with the care of cardiac arrest patients; specifically emergency medicine, internal medicine (divisions of cardiology and pulmonary and critical care medicine), neurology, cardiothoracic surgery and neurosurgery. At the same time, the education program was further expanded to the local community of emergency medical service (EMS) providers in collaboration with Edward Stapleton, an associate professor in the emergency department, in order to ensure that any patient who suffers a cardiac arrest whether in the community or within the hospital can receive enhanced care. This monthly training and education program consistently received very high feedback scores from participants. The main goal of the two parallel education programs has been to educate all staff involved with cardiac arrest care regarding the importance of effective CPR delivery with a particular focus on brain and other vital organ oxygen delivery. This novel and critical component of the education program has been an entirely new innovation in the US. Our program also included education regarding the importance and methods for delivering standardized post-resuscitation care for patients for up to 72 hours after restoration of the heartbeat after CPR.
The education component has been disseminated with the help of other key members and in particular Dr. Barbara Mills (Director of Rapid Response Service) and Dr. Sahar Ahmed (Faculty in Pulmonary & Critical Care). This has been an on-going program in which medical residents and critical care fellows receive enhanced training through a combination of didactic and simulation methods. These efforts were combined with focused lectures, meetings and discussion with hospital leadership, nursing leadership and key faculty in all the divisions and departments involved with the care of cardiac arrest patients; specifically emergency medicine, internal medicine (divisions of cardiology and pulmonary and critical care medicine), neurology, cardiothoracic surgery and neurosurgery. At the same time, the education program was further expanded to the local community of emergency medical service (EMS) providers in collaboration with Edward Stapleton, an associate professor in the emergency department, in order to ensure that any patient who suffers a cardiac arrest whether in the community or within the hospital can receive enhanced care. This monthly training and education program consistently received very high feedback scores from participants. The main goal of the two parallel education programs has been to educate all staff involved with cardiac arrest care regarding the importance of effective CPR delivery with a particular focus on brain and other vital organ oxygen delivery. This novel and critical component of the education program has been an entirely new innovation in the US. Our program also included education regarding the importance and methods for delivering standardized post-resuscitation care for patients for up to 72 hours after restoration of the heartbeat after CPR.
Incorporation of Technology to Advance Patient Care
 Starting in 2011 at Stony Brook Medical Center, novel technology was introduced in a highly cost effective manner for the clinical practice of resuscitation. In particular, a series of five “Supplementary Mobile Resuscitation Carts” were created and housed in strategic locations within the hospital (coronary care unit, medical ICU, emergency department), these are immediately taken to the scene of cardiac arrest, irrespective of hospital location. The carts include an automated-CPR device, portable ultrasound, an intraosseous device, end tidal CO2 monitoring, quality-CPR monitoring as well as and real time brain monitoring of the level of oxygen being delivered during CPR. These carts are still routinely in use at the institution on a 24/7 basis.
Starting in 2011 at Stony Brook Medical Center, novel technology was introduced in a highly cost effective manner for the clinical practice of resuscitation. In particular, a series of five “Supplementary Mobile Resuscitation Carts” were created and housed in strategic locations within the hospital (coronary care unit, medical ICU, emergency department), these are immediately taken to the scene of cardiac arrest, irrespective of hospital location. The carts include an automated-CPR device, portable ultrasound, an intraosseous device, end tidal CO2 monitoring, quality-CPR monitoring as well as and real time brain monitoring of the level of oxygen being delivered during CPR. These carts are still routinely in use at the institution on a 24/7 basis.
During this time, a comprehensive post-resuscitation management program was also created as well as a dedicated quality reporting dashboard relating to both intra cardiac arrest and post resuscitation (ICU) variables. The Stony Brook Post-Resuscitation dashboard was created approximately 12-24 months before a similar dashboard was introduced by the American Heart Association’s “Get With The Guidelines - Resuscitation” program.