With a reputation as a leading authority on pain management, the Center for Pain Management at Stony Brook University Medical Center has served Long Island since 1982. Our program uses the biopsychosocial model of medicine to treat chronic and acute pain, provide palliative care, and improve the functionality and quality of life of our patients. We work in partnership with area physicians to offer consultations, diagnoses, plans of treatment and multidisciplinary care before returning the patient to his or her primary care doctor.
In 2023, the Stony Brook Center for Pain Management moved to the Advanced Specialty Care Pavilion in Lake Grove at the Smith Haven Mall. It is Stony Brook Medicine’s newest and most spacious, multispecialty care facility. Featuring a modern, open-concept layout, occupying approximately 170,000 square feet, our new office more than doubles the square footage of our prior office. The office is equipped with 9 exam rooms, 3 fully functional fluoroscopy suites, and an 8 bay PACU area. The increased space was vital to accommodate our growing clinical practice and to continue to improve the educational experience for our medical students, residents, and fellows.
In 2023, the Stony Brook Center for Pain Management moved to the Advanced Specialty Care Pavilion in Lake Grove at the Smith Haven Mall. It is Stony Brook Medicine’s newest and most spacious, multispecialty care facility. Featuring a modern, open-concept layout, occupying approximately 170,000 square feet, our new office more than doubles the square footage of our prior office. The office is equipped with 9 exam rooms, 3 fully functional fluoroscopy suites, and an 8 bay PACU area. The increased space was vital to accommodate our growing clinical practice and to continue to improve the educational experience for our medical students, residents, and fellows.
Division Members
 Assistant Professor Director: Center for Pain Management Chief of the Chronic Pain Division |
 Assistant Professor Director: Stony Brook Pain Medicine Fellowship Program |
|
 Assistant Professor |
 Assistant Professor |
|
 |
 |
|
Residency Training
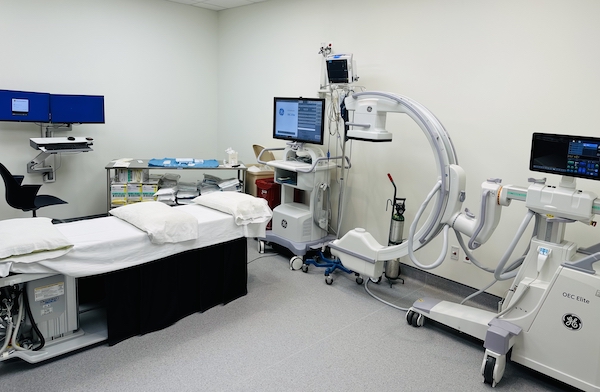
There is an in-office fluoroscopy suite for epidural, facet, major joint, peripheral nerve blocks, and sympathetic nerve block procedures. Ultrasound guided injections are also utilized. Residents will also be exposed to traditional spinal cord stimulation, as well as dorsal root ganglion stimulation and other treatment modalities such as Botox and IV infusion therapies.
Trainees will greatly expand their knowledge base, skills, and judgment so that they can recognize and manage complications associated with chronic pain. Residents receive hands on training to give them the skills necessary for their fellowship and future careers.
- The CA-2 rotation is a one month rotation. [Pain Rotation Primer]
- The three month elective in the CA-3 year is structured as a "mini-fellowship". Residents on the rotation will participate in journal club presentations and receive several core lectures. [CA-3 Mini-Fellowship]
-
▶ The life of a Resident on the Chronic Pain Rotation ...
Recent Division Activity
 |
 |
|
 |
 |
Recent Publications
Resident authors denoted by bold type
- Gupta AK, Mena S, Jin Z, Gan TJ, Bergese SD. Postoperative pain: a review of emerging therapeutic options. Expert Rev Neurother. 2021 Aug 31
- Desai A, Dahan A, Gan TJ. Perioperative Opioid Education Initiatives: Do They Add Value? Anesth Analg. 2022 May 1;134(5):938-939.
- Palaniappan D, Friedlander D, Desai A. Is it time to reconsider the routine blind insertion of double lumen endobronchial tubes? J Clin Anesth. 2022 Aug;79:110766.
- Ghaly L, Bargnes V, Rahman S, Tawfik GA, Bergese S, Caldwell W. Interventional Treatment of Complex Regional Pain Syndrome. Biomedicines. 2023 Aug 14;11(8):2263
- Rahman S, Kidwai A, Rakhamimova E, Elias M, Caldwell W, Bergese SD. Clinical Diagnosis and Treatment of Chronic Pain. Diagnostics (Basel). 2023 Dec 18;13(24):3689.
- Wang A, Murphy J, Shteynman L, Daksla N, Gupta A, Bergese S. Novel Opioids in the Setting of Acute Postoperative Pain: A Narrative Review. Pharmaceuticals (Basel). 2023 Dec 25;17(1):29.
- Burjek NE, Hafeman M, Guthrie D, Desai A, Jin Z, Brockel M, Moore R. Perioperative use of gabapentinoids in pediatric patients. APS 2023:1, 21.
- Wang A, Kerolus K, Garry E, Li D, Desai A, Bergese S. Novel Techniques and Local Anesthetics for Perioperative Pain Management. In: Advances in Regional Anesthesia. Rijeka: IntechOpen; 2023.
- Mena S, Raj A, Caldwell W, Kaushal A. The annoyance of singultus: a case report of a rare adverse effect after epidural steroid injection. BMC Anesthesiol. 2024 Aug 31;24(1):302.
- Desai A, Razak A, Ghaly L, Bennici L, Moore R. Opioid-Obviating Analgesia for Adolescent Multilevel Spinal Fusion Surgery: A Problem-Based Learning Discussion. A A Pract. 2024 Jul 11;18(7):e01823.
- Kirsch E, Rahman S, Kerolus K, Hasan R, Kowalska DB, Desai A, Bergese SD. Dysmenorrhea, a Narrative Review of Therapeutic Options. J Pain Res. 2024 Aug 15;17:2657-2666.
- Lee E, Kim J, Rahman S, Daksla N, Caldwell W, Bergese S. Basivertebral Nerve Ablation for Treatment of Lower Back Pain. Biomedicines. 2024 Sep 9;12(9):2046
- Torpey A, Bellow E, Samojedny V, Ahluwalia S, Desai A, Caldwell W, Bergese S. Nanotechnology in Pain Management. Pharmaceutics. 2024 Nov 20;16(11):1479
- Greenspan S, Torpey A, Desai A. Fellowship or Not, We Are All Pain Physicians. ASA Monitor 2025 89(3), 35
- Xie S, Bindelglass A, Moore RP, Desai A. Erector spinae nerve blocks for use in proximal humeral fractures surgery: Two case reports. JCA Advances 2025 2(1)
- Zimmerman AJ, Mangano N, Park G, Kaushal AK, Bergese SD. Glial Modulator Antibiotics for Neuropathic Pain: Current Insights and Future Directions. Pharmaceuticals. 2025; 18(3):346
Recent Presentations
- Mena S, Parikh S, Desai A. Neuraxial Analgesia For A Sacral Decubitus Ulcer. PGA 2021
- Kang R, Shuaib K, Parikh S, Desai A. Epidural Analgesia For Chemical Pleurodesis. PGA 2021
- Mena S, Kang RS, Caldwell W. Spinal Cord Stimulation for Sciatic Pain in Seronegative Neuromyelitis Optica Spectrum Disorder. IARS 2022
- Mena S, Kang RS, Caldwell W. Spinal Cord Stimulation for Sciatic Pain in Seronegative Neuromyelitis Optica Spectrum Disorder. ASA 2022
- Elias M, Kang RS, Kaushal AK. Treatment of Umbilical Hernia Pain with Ultrasound-guided Abdominal Botox Injections. ASA 2022
- Hafeman M, Desai AG, Moore RP. High Thoracic Erector Spinae Plane (ESP) Block for Humeral Osteotomy. ASA 2022
- Kozlowski P, Turkiew E, Desai AG, Bennici LA, Moore RP. Opioid Free Thoracolumbar Fusion in a Pediatric Patient with a Polysubstance Abuse History. ASA 2022
- Ghaly L, Zimmerman A, Kaushal A. The use of stellate ganglion block for post- covid-19 pleuritic chest pain. ASRA 2023
- Rahman S, Desai A, Moore R. Erector spinae plane block for cancer related brachial plexus pain - A new role for regional anesthesia in NORA? ASRA 2023
- Rahman S, Desai A, Moore R. Erector spinae block for NORA to treat selective brachial plexus pain in patient with metastatic lung cancer. PGA 2023
- Greenspan S, Gordon J, Oo J, Caldwell W. Combined Basivertebral Nerve Ablation and Interspinous Spacer Implants Provides Effective Long-term Pain Relief in a Patient with Severe Low Back and Leg Pain. ASA 2024
- Mangano N, De La Hoz M, Oo J, Caldwell W. Basivertebral Nerve Ablation and Spinal Cord Stimulation for Successful Management of Lower Back and Radicular Leg Pain Refractory to Spinal Fusion Surgery. ASA 2024
- Zimmerman AJ, Oo J, Chikvashvii D, Caldwell W. Combined Basivertebral Nerve Ablation and Interspinous Spacer Implants Provides Effective Long-Term Pain Relief for Severe Radicular Low Back Pain: A Case Report. NY NJ Pain Medicine Congress 2024
- Zimmerman AJ, Kordic N, Cohen E, Caldwell W. Combined Basivertebral Nerve Ablation and Spinal Cord Stimulation Provides Effective Long-Term Pain Relief in Failed Back Surgery Syndrome: A Case Report. NY NJ Pain Medicine Congress 2024
- Zimmerman AJ, Zektser K, Cohen E, Caldwell W. Inability to Wear Sandals and Heels: A Rare Case and Treatment for Dorsal Medial Foot Pain. NY NJ Pain Medicine Congress 2024
- Rahman S, Rismany J, Caldwell W. Basivertebral Nerve Ablation as An Effective Treatment for Chronic Lower Back Pain after Spinal Fusion Surgery for Scoliosis. NY NJ Pain Medicine Congress 2024
- Rahman S, Bhimavarapu A, Desai A. Management of Chronic Pain associated with Small Fiber Neuropathy Secondary to SARS-CoV-2. ASA 2024
- Rahman S, Bhimavarapu A, Desai A. Management of Chronic Pain associated with Small Fiber Neuropathy Secondary to SARS-CoV-2. PGA 2024
- Charkowick S, Weng A, Bargnes V, Nada E, Desai A. Don’t Get Caught in the Web: A Multicatheter Approach to Treat Bilateral Rib Fractures in the Setting of a Thoracic Arachnoid Web. ASRA 2025
faculty photos by Jeanne Neville