The Division of Regional Anesthesia is under the direction of Dr. Eman Nada. The team works closely with surgeons to assure that the patients' entire perioperative experience is pleasant.
Stony Brook University Hospital is one of the largest Trauma Centers in the nation, thereby allowing residents to participate in providing safe and effective anesthesia care to orthopedic trauma, which encompasses spinal fractures, acetabulum, pelvic fractures and multiple extremity fractures. This includes patients with unstable cervical spinals requiring advanced airway management techniques and advanced fluid and coagulation management strategies. The Division of Regional Anesthesia also serves a large patient population requiring total joint replacement, adult spine surgery, elective orthopedic trauma surgery, sports medicine, hand surgery and a variety of plastic surgeries. The Division includes regional anesthesiologists trained in the delivery of state-of-the-art neuroaxial and peripheral nerve blocks for improved patient care. The Division is proud to have participated in the care of patients who have had both hands reattached in an eleven-hour surgical procedure after an industrial accident. This case gained both national and international publicity, demonstrating the excellence of care provided here at Stony Brook University Hospital.
Stony Brook University Hospital is one of the largest Trauma Centers in the nation, thereby allowing residents to participate in providing safe and effective anesthesia care to orthopedic trauma, which encompasses spinal fractures, acetabulum, pelvic fractures and multiple extremity fractures. This includes patients with unstable cervical spinals requiring advanced airway management techniques and advanced fluid and coagulation management strategies. The Division of Regional Anesthesia also serves a large patient population requiring total joint replacement, adult spine surgery, elective orthopedic trauma surgery, sports medicine, hand surgery and a variety of plastic surgeries. The Division includes regional anesthesiologists trained in the delivery of state-of-the-art neuroaxial and peripheral nerve blocks for improved patient care. The Division is proud to have participated in the care of patients who have had both hands reattached in an eleven-hour surgical procedure after an industrial accident. This case gained both national and international publicity, demonstrating the excellence of care provided here at Stony Brook University Hospital.
Division Members
 Chief of Regional Anesthesia |
- Eman Nada, MD, PhD is an Associate Professor and Chief of the Division. Before joining our department in June 2021, Dr. Nada did Fellowship training in Neuroanesthesia and Regional Anesthesia/Acute Pain at the Cleveland Clinic.
- Ramon Abola, MD is the Director of Communication and Deputy Chief Medical Information Officer, Stony Brook Medicine. He is an Associate Editor for BMC Anesthesiology.
- Syed Azim, MD is an Associate Professor and has an interest in the mechanisms of pain after knee surgery.
- Lesley Bennici, MD joined our department in 2018 after an Anesthesia Residency at New York University School of Medicine.
- Amruta Desai, DO, MBA, MPH joined our department in January 2021 after doing a fellowship in Pain Medicine at UMass Medical School.
- Michelle DeLemos, MD serves as the Assistant Residency Program Director for the department.
- Xiaojun Guo, MD, FASA. Dr. Guo splits his time between the NORA and Regional Anesthesia divisions. His main areas of interest in acupuncture are Influenza prevention and preoperative sedation with acupuncture.
- Jun Lin, MD, PhD, FASA directs an externally funded research program "Cancer Recurrence and Metastasis following Surgery and Anesthesia".
- Sun Mei Liu, MD.
- Meng Wang, MD, PhD has a doctorate in Neuroscience and is also a member of the General Anesthesia Division.
Residency Training
CA1 residents have a 4-week mandatory rotation closely supervised by the faculty in the division. Typically, residents receive a welcoming e-mail from our educational director explaining what to expect during this rotation, detailed goals and objectives, and a list of the topics needed to be discussed intraoperatively with the faculty during the rotation. We place a lot of emphasis on intraoperative teaching. There is also an exit quiz/ test at the end of the rotation.
This rotation also offers a great learning opportunity for the residents, as the nature of the cases are different every day since our patient population is diverse. Cases could range from an elderly patient with many co-morbidities having a fragility hip fracture to a penetrating multiple Ortho trauma needed advanced airway technique or to manage a complex trauma patient involving multiple specialties with pelvic fracture, to a simple sports-related knee arthroscopy or elective joint replacement, spine and breast surgery.
The residents are also exposed to variety of acute pain procedures, and learn how to manage the acute postoperative pain.
This rotation also offers a great learning opportunity for the residents, as the nature of the cases are different every day since our patient population is diverse. Cases could range from an elderly patient with many co-morbidities having a fragility hip fracture to a penetrating multiple Ortho trauma needed advanced airway technique or to manage a complex trauma patient involving multiple specialties with pelvic fracture, to a simple sports-related knee arthroscopy or elective joint replacement, spine and breast surgery.
The residents are also exposed to variety of acute pain procedures, and learn how to manage the acute postoperative pain.
Recent Division Activity
The REGAIN trial has been completed. The results were published in The New England Journal of Medicine. REGAIN, a Multicenter randomized controlled trial which compares survival, functional recovery, cognitive outcomes and postoperative adverse events among patients age 50 and older receiving spinal vs GA for hip fracture surgery.
 |
 |
Recent Publications
Resident authors denoted by bold type
- Neuman MD, Feng R, Carson JL, Gaskins LJ, Dillane D, Sessler DI, Sieber F, Magaziner J, Marcantonio ER, Mehta S, Menio D, Ayad S, Stone T, Papp S, Schwenk ES, Elkassabany N, Marshall M, Jaffe JD, Luke C, Sharma B, Azim S, Hymes RA, Chin KJ, Sheppard R, Perlman B, Sappenfield J, Hauck E, Hoeft MA, Giska M, Ranganath Y, Tedore T, Choi S, Li J, Kwofie MK, Nader A, Sanders RD, Allen BFS, Vlassakov K, Kates S, Fleisher LA, Dattilo J, Tierney A, Stephens-Shields AJ, Ellenberg SS; REGAIN Investigators. Spinal Anesthesia or General Anesthesia for Hip Surgery in Older Adults. N Engl J Med. 2021 Oct 9.
- Jin Z, Zhu M, Gupta A, Page C, Gan TJ, Bergese SD. Evaluating oliceridine as a treatment option for moderate to severe acute post-operative pain in adults. Expert Opin Pharmacother. 2021 Sep 17.
- Liu Q, Li R, Li Q, Luo B, Lin J, Lyu L. High levels of plasma S100A9 at admission indicate an increased risk of death in severe tuberculosis patients. J Clin Tuberc Other Mycobact Dis. 2021 Sep 13;25:100270.
- Desai A, Dahan A, Gan TJ. Perioperative Opioid Education Initiatives: Do They Add Value? Anesth Analg. 2022 May 1;134(5):938-939.
- Palaniappan D, Friedlander D, Desai A. Is it time to reconsider the routine blind insertion of double lumen endobronchial tubes? J Clin Anesth. 2022 Aug;79:110766.
- Liu Q, Li R, Lin J. No Difference Among Inhaled Anesthetics on the Growth and Metastasis of Murine 4T1 Breast Cancers in a Mouse Model of Spontaneous Metastasis. Front Pharmacol. 2022 Feb 9;13:794109.
- Jin Z, Zhang W, Liu H, Ding A, Lin Y, Wu SX, Lin J. Potential Therapeutic Application of Local Anesthetics in Cancer Treatment. Recent Pat Anticancer Drug Discov. 2022 Jan 19.
- Li R, Mukherjee MB, Lin J. Coordinated Regulation of Myeloid-Derived Suppressor Cells by Cytokines and Chemokines. Cancers (Basel). 2022 Feb 27;14(5):1236.
- Chang JL, Goldberg AN, Alt JA, Ashbrook L, Auckley D, Ayappa I, Bakhtiar H, Barrera JE, Bartley BL, Billings ME, Boon MS, Bosschieter P, Braverman I, Brodie K, Cabrera-Muffly C, Caesar R, Cahali MB, Cai Y, Cao M, Capasso R, Caples SM, Chahine LM, Chang CP, Chang KW, Chaudhary N, Cheong CSJ, Chowdhuri S, Cistulli PA, Claman D, Collen J, Coughlin K, Creamer J, Davis EM, Dupuy-McCauley KL, Durr ML, Dutt M, Ali ME, Elkassabany NM, Epstein LJ, Fiala JA, Freedman N, Gill K, Gillespie MB, Golisch L, Gooneratne N, Gottlieb DJ, Green KK, Gulati A, Gurubhagavatula I, Hayward N, Hoff PT, Hoffmann OMG, Holfinger SJ, Hsia J, Huntley C, Huoh KC, Huyett P, Inala S, Ishman S, Jella TK, Jobanputra AM, Johnson AP, Junna MR, Kado JT, Kaffenberger TM, Kapur VK, Kezirian EJ, Khan M, Kirsch DB, Kominsky A, Kryger M, Krystal AD, Kushida CA, Kuzniar TJ, Lam DJ, Lettieri CJ, Lim DC, Lin HC, Liu SYC, MacKay SG, Magalang UJ, Malhotra A, Maurer JT, May AM, Mitchell RB, Mokhlesi B, Mullins AE, Nada EM, Naik S, Nokes B, Olson MD, Pack AI, Pang EB, Pang KP, Patil SP, de Perck EV, Piccirillo JF, Pien GW, Piper AJ, Plawecki A, Quigg M, Ravesloot MJL, Redline S, Rotenberg BW, Ryden A, Sarmiento KF, Sbeih F, Schell AE, Schmickl CN, Schotland HM, Schwab RJ, Seo J, Shah N, Shelgikar AV, Shochat I, Soose RJ, Steele TO, Stephens E, Stepnowsky C, Strohl KP, Sutherland K, Suurna MV, Thaler E, Thapa S, Vanderveken OM, de Vries N, Weaver EM, Weir ID, Wolfe LF, Woodson BT, Won CHJ, Xu J, Yalamanchi P, Yaremchuk K, Yeghiazarians Y, Yu JL, Zeidler M, Rosen IM. International consensus statement on obstructive sleep apnea. Int Forum Allergy Rhinol. 2022 Sep 6.
- Qureshi F, Romeiser JL, Murphy PF, Go R, Abola R. A Quality Assurance Initiative on Improving Cefazolin Peri-operative Redose Compliance. Int J Qual Health Care. 2022 Sep 14.
- Palaniappan D, Friedlander D, Desai A. Is it time to reconsider the routine blind insertion of double lumen endobronchial tubes? J Clin Anesth. 2022 Aug;79:110766.
- Scorsese G, Jin Z, Greenspan S, Seiter C, Jiang Y, Huang MB, Lin J. Effectiveness of Thoracic Wall Blocks in Video-Assisted Thoracoscopic Surgery, a Network Meta-Analysis. J Pain Res. 2023 Mar 7;16:707-724.
- O'Brien K, Feng R, Sieber F, Marcantonio ER, Tierney A, Magaziner J, Carson JL, Dillane D, Sessler DI, Menio D, Ayad S, Stone T, Papp S, Schwenk ES, Marshall M, Jaffe JD, Luke C, Sharma B, Azim S, Hymes R, Chin KJ, Sheppard R, Perlman B, Sappenfield J, Hauck E, Hoeft MA, Karlawish J, Mehta S, Donegan DJ, Horan A, Ellenberg SS, Neuman MD; REGAIN (Regional versus General Anesthesia for Promoting Independence after Hip Fracture) Investigators. Outcomes with spinal versus general anesthesia for patients with and without preoperative cognitive impairment: Secondary analysis of a randomized clinical trial. Alzheimers Dement. 2023 May 12.
- Li R, Mukherjee MB, Jin Z, Liu H, Lin K, Liu Q, Dilger JP, Lin J. The Potential Effect of General Anesthetics in Cancer Surgery: Meta-Analysis of Postoperative Metastasis and Inflammatory Cytokines. Cancers (Basel). 2023 May 15.
- Vail EA, Feng R, Sieber F, Carson JL, Ellenberg SS, Magaziner J, Dillane D, Marcantonio ER, Sessler DI, Ayad S, Stone T, Papp S, Donegan D, Mehta S, Schwenk ES, Marshall M, Jaffe JD, Luke C, Sharma B, Azim S, Hymes R, Chin KJ, Sheppard R, Perlman B, Sappenfield J, Hauck E, Tierney A, Horan AD, Neuman MD; REGAIN (Regional versus General Anesthesia for Promoting Independence after Hip Fracture) Investigators. Long-term outcomes with spinal versus general anesthesia for hip fracture surgery: A randomized trial. Anesthesiology. 2023 Oct 13.
- Burjek NE, Hafeman M, Guthrie D, Desai A, Jin Z, Brockel M, Moore R. Perioperative use of gabapentinoids in pediatric patients. APS 2023:1, 21.
- Jin Z, Bargnes V, Tsivitis A, Oster J, Lin J. Palliative Care Surgery of Cancer Patients. 2023. In: Huang J, Huang J, Liu H. (eds) Anesthesia for Oncological Surgery. Springer, Cham.
- Wang A, Kerolus K, Garry E, Li D, Desai A, Bergese S. Novel Techniques and Local Anesthetics for Perioperative Pain Management. In: Advances in Regional Anesthesia (ed. Hurtado EDM). IntechOpen, Publisher 2024.
- Desai A, Razak A, Ghaly L, Bennici L, Moore R. Opioid-Obviating Analgesia for Adolescent Multilevel Spinal Fusion Surgery: A Problem-Based Learning Discussion. A A Pract. 2024 Jul 11;18(7):e01823.
- Kirsch E, Rahman S, Kerolus K, Hasan R, Kowalska DB, Desai A, Bergese SD. Dysmenorrhea, a Narrative Review of Therapeutic Options. J Pain Res. 2024 Aug 15;17:2657-2666.
Recent Presentations
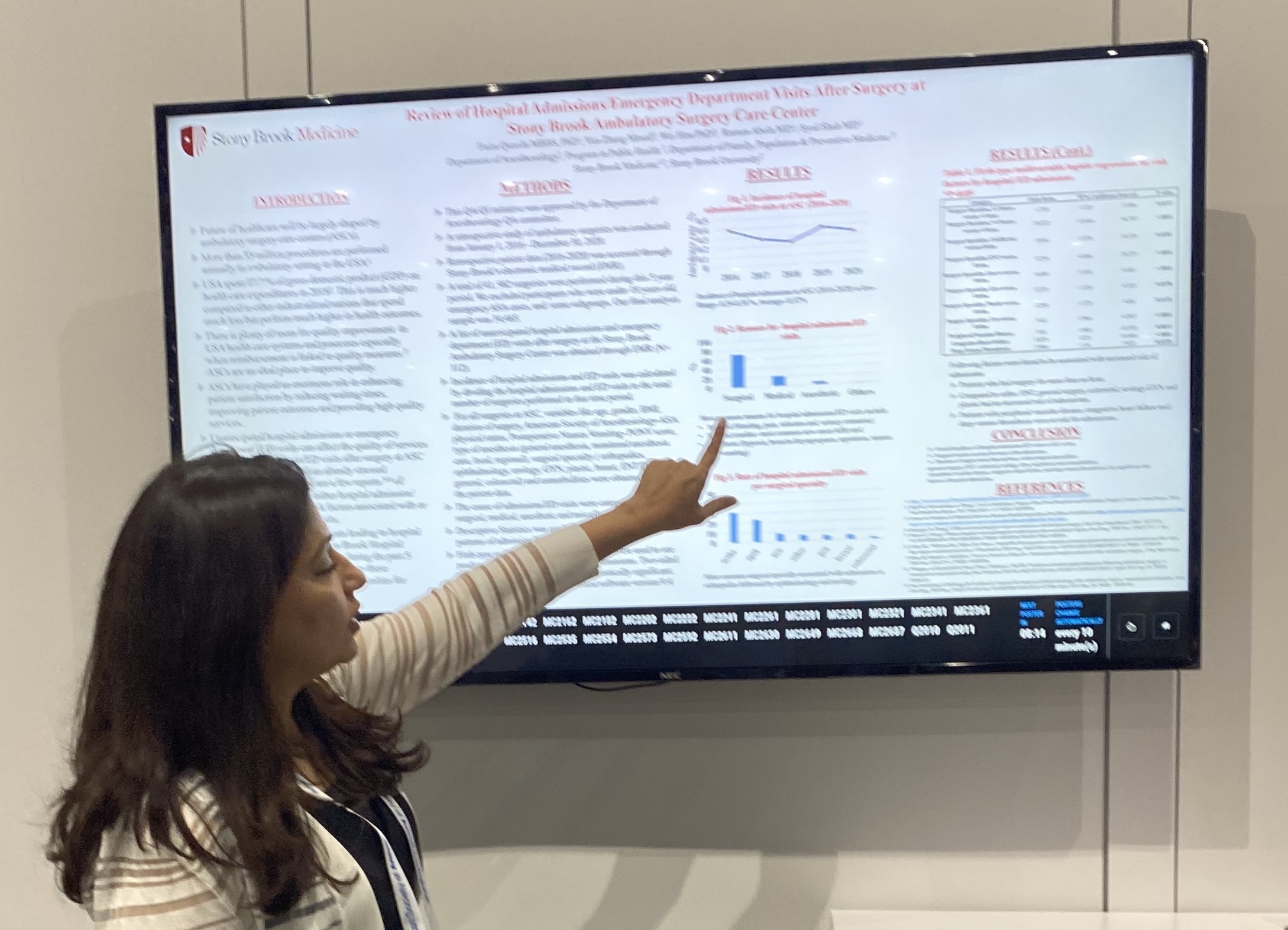
- Qureshi F, Abola R, Shah A. Review of Hospital Admissions Emergency Department Visits after Surgery at Stony Brook Ambulatory Surgery Care Center. ASA 2021
- Qureshi F, Abola R. Peri-induction Cardiac Arrest Review. ASA 2021
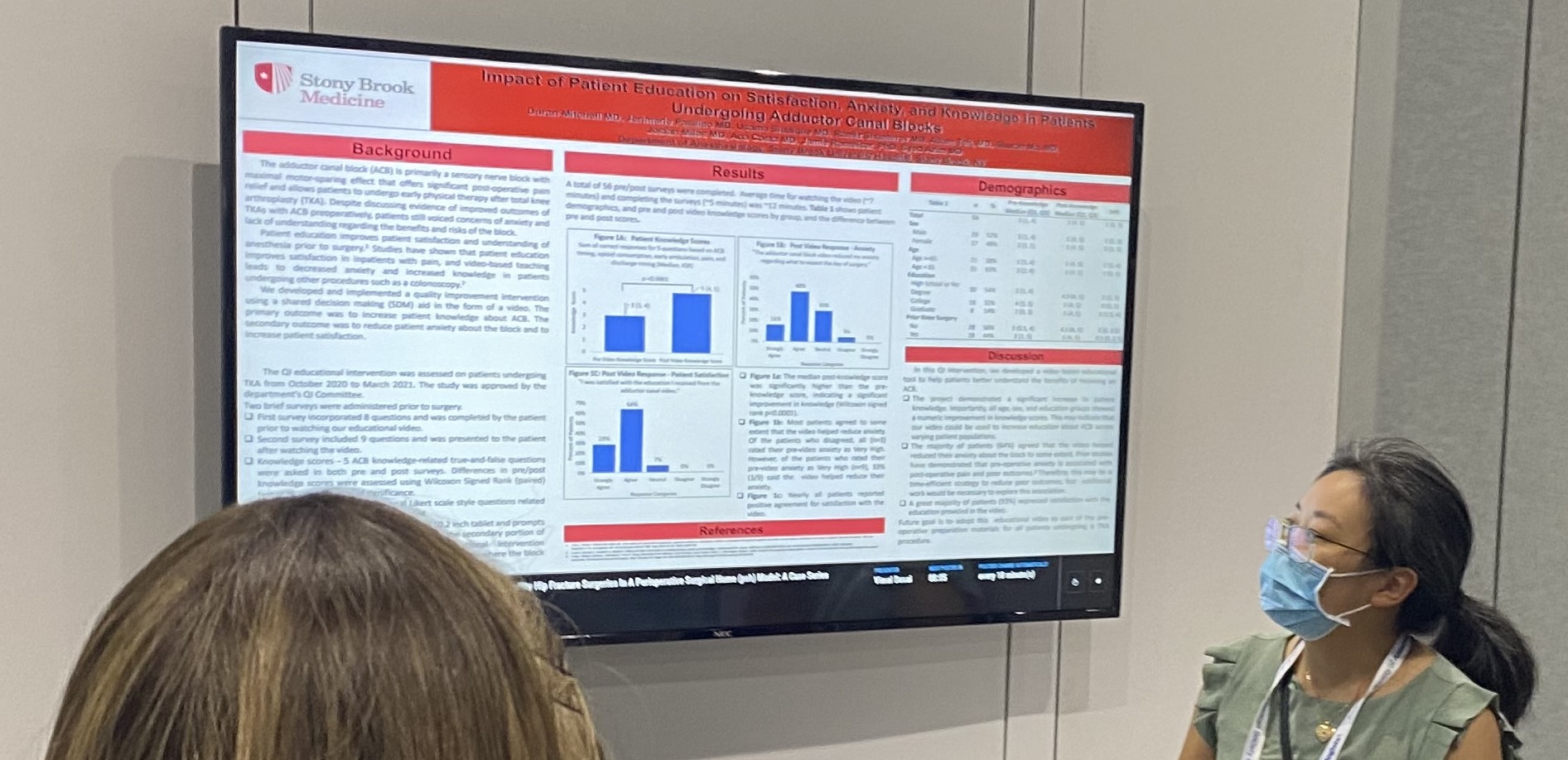
- Mitchell D, Pasillao J, Siddique U, Shuminov R, Taft A, Ma S, Miles J, Costa A, Romeiser J, Azim S. Impact of Patient Education on Satisfaction, Anxiety, and Knowledge in Patients Undergoing Adductor Canal Blocks. ASA 2021
- Kang RS, Nguyen CP, Bennici LA. Perioperative Management Of Autoimmune Polyglandular Syndrome Type 1. ASA 2021
- Mena S, Desai A. Pain Management in a Parturient on Suboxone with a Complex Right Hip Fracture. ASA 2021
- Shafai A, Desai A. To decrease or continue high dose buprenorphine period. ASA 2021
- Mena S, Gruttadauria M, Factor M, DeLemos M. Spinal Anesthesia in Suspected Brugada Syndrome. ASA 2021
- Costa A, Chandran L, Schabel J, Abola R, Fischel J. Practice Habits And Data Analytics In Anesthesiology Resident Education. PGA 2021
- Shuaib K, Kang RS, Bennici L. A Pediatric Patient With Erythromelalgia. PGA 2021
- Mena S, Parikh S, Desai A. Neuraxial Analgesia For A Sacral Decubitus Ulcer. PGA 2021
- Kang R, Shuaib K, Parikh S, Desai A. Epidural Analgesia For Chemical Pleurodesis. PGA 2021
- Li R, Jin Z, Lin J. Combined general/epidural anesthesia vs general anesthesia on the postoperative inflammation or stress response: a systemic review and meta-analysis. PGA 2021
- Jin Z, Li R, Lin J. Intravenous vs volatile anesthesia and colorectal cancer surgery outcome - a systematic review and meta-analysis. PGA 2021
- Lin J, Jin Z, Tai J. Tumor recurrence following postoperative infection - a systematic review. IARS 2022
- Scorsese G, Jiang Y, Greenspan SH, Jin Z, Seiter C, Kianian S, Lin J. The Efficacy of Serratus Anterior Plane Block for Postoperative Analgesia after Video-Assisted Thorascopic Surgery. IARS 2022
- Lin J, Li R, Jin Z, Liu Q, Ding O, Jiang Y. Effect of epidural anesthesia on postoperative inflammation or stress response: a systematic review and meta-analysis. IARS 2022
- Seiter C, Jin Z, Scorsese G, Jiang Y, Greenspan SH, Lin J. Erector Spinae Plane Block for Postoperative Analgesia after Video Assisted Thorascopic Surgery. IARS 2022
- Shafai A, Nada E. The Use of External Oblique Intercostal Nerve Block for Post-operative Pain Control in a Patient Undergoing Radical Nephrectomy. ASA 2022
- Zhu M, Nada E. Application of Fascia Plane Blocks for Subcutaneous Implantable Defibrillator Pain. ASA 2022
- Qureshi F, Zhang X, Abola RE. Implementation of Automated Reporting of Anesthesia Quality Measures-phase 1. ASA 2022
- Zhu M, Kozlowski P, Jin Z, Azim SA, Gan TJ. Recovery after Spinal Anesthesia with Mepivacaine vs Bupivacaine, A Systematic Review and Meta-analysis. ASA 2022
- Singh S, Azim SA, Murtha C, Walsh L, Antonelli L, Hoffman D, Nicholson J, Bennett-Guerrero E. Using an ERAS Joint Replacement Pathway To Improve Urinary Management in Elective Surgical Patients. ASA 2022
- Singh S, Azim SA, Murtha C, Walsh L, Antonelli L, Hoffman D, Nicholson J, Bennett-Guerrero E. Adapting our Total Joint Replacement Enhanced Recovery after Surgery Program to Improve Surgical Care During a Pandemic. ASA 2022
- Hafeman M, Desai AG, Moore RP. High Thoracic Erector Spinae Plane (ESP) Block for Humeral Osteotomy. ASA 2022
- Kozlowski P, Turkiew E, Desai AG, Bennici LA, Moore RP. Opioid Free Thoracolumbar Fusion in a Pediatric Patient with a Polysubstance Abuse History. ASA 2022
- Ahn J, Jin Z, Cuenca J, Lin J, Gan TJ. Quadratus Lumborum Block for Analgesia after Renal Surgeries - A Systematic Review and Meta-analysis. ASA 2022
- Jin Z, Greenspan S, Jiang Y, Seiter C, Scorsese , Lin J. Thoracic Paravertebral Block Versus Erector Spinae Block for Postoperative Analgesia after Video Assisted Thoracoscopic Surgery. ASA 2022
- Hafeman M, Jiang Y, Jin Z, Seiter C, Scorsese GF, Greenspan S, Lin J. Thoracic Epidural vs. Continuous Paravertebral Block for Analgesia after VATS: a Meta-analysis. ASA 2022
- Cuenca J, Jin Z, Ahn J, Poovathoor SP, Lin J. Efficacy of Remimazolam for Procedural Sedation Compared to Midazolam - A Systematic Review and Meta-analysis. ASA 2022
- Elias M, Nada E. Venous Air Embolism In Patient Undergoing Hemodialysis Catheter Placement. PGA 2022
- Jin Z, Rakhamimova E, Lin J, Nada E. Comparison of liposomal bupivacaine to conventional local anesthetics in adductor canal block for knee surgery, a meta-analysis. IARS 2023v
- Mattimore D, Nada E. External Oblique Intercostal Nerve Block after Radical Nephrectomy with IVC or Renal Vein Thrombectomy. ASRA 2023
- Ghaly L, Nada E. A Case of Propofol-Induced Myoclonus During Short-Term Infusion with Regional Anesthesia. ASRA 2023
- Rahman SDesai A, Moore R. Erector spinae plane block for cancer related brachial plexus pain - A new role for regional anesthesia in NORA? ASRA 2023
- Bell J, Azim SA. Post Operative Vision Loss in a Twelve Year Old Following Spine Surgery. ASA 2023
- Lin J, Mousumi M, Mukherjee M, Jin Z, Li R. Systemic Review and Meta-analysis of Postoperative Inflammatory Cytokines in Cancer Surgery Under Inhaled or Intravenous Anesthetics. ASA 2023
- Lin J, Jin Z, Mousumi B, Mukherjee MB, Li R. The Potential Role of General Anesthetics in Cancer Surgery: Meta-analysis of Postoperative Metastasis. ASA 2023
- Elias M, Zhu M, Liu SM. Management of a Difficult Airway in a Patient with Advanced Head and Neck Sarcoma. ASA 2023
- Razak A, Murphy J, Jin Z, Wang M. Efficacy of Liposomal Bupivacaine Versus Local Anesthetics in Transversus Abdominis Plane Blocks: A Meta-analysis. ASA 2023
- Chen X, Raj A, Oleszak SP, Wang M. Stridor and Cervical Fracture: Worst Combination in Airway Management. ASA 2023
- Murphy J, Razak A, Jin Z, Wang M. Efficacy Of Liposomal Bupivacaine Versus Local Anesthetics In Transversus Abdominis Plane Blocks: A Meta-analysis. PGA 2023
- Rakhamimova E, Jin Z, Lin J. Comparison of liposomal bupivacaine to conventional local anesthetics in adductor canal block for knee surgery, a meta-analysis. PGA 2023
- Doudnikoff A, Mangano N, Patel S, Razak A, Nada E. Assessing pain in the setting of dementia in an elderly patient with rib fractures. PGA 2023
- Rahman S, Desai A, Moore R. Erector spinae block for NORA to treat selective brachial plexus pain in patient with metastatic lung cancer. PGA 2023
- Razak A, Kerolus K, Aravera C, Liu SM, Wang M, Nada E. The Utility of Epidural Analgesia for Acetabular Fractures in Trauma Patients: A Case Report. ASRA Spring 2024
- Razak A, Wozniak S, Nada E. Retroclavicular Approach to the Infraclavicular Region Nerve Block in a Patient with an Upper Extremity Burn Injury. ASRA Spring 2024