| About | Members | Resident Training | Patient Care |
| Fellowship | Recent Activity | Publications | Presentations |
Women's Anesthesia Division
 We are thrilled to announce that the Division of Obstetric Anesthesiology at Stony Brook has been designated as a Center of Excellence by the Society of Obstetric Anesthesia and Perinatology since 2021.
We are thrilled to announce that the Division of Obstetric Anesthesiology at Stony Brook has been designated as a Center of Excellence by the Society of Obstetric Anesthesia and Perinatology since 2021.
The SOAP Center of Excellence (COE) designation was created to recognize institutions and programs that demonstrate excellence in obstetric anesthesia care and to set a benchmark of expected care to improve standards nationally and internationally. The criteria cover all aspects of obstetric anesthesia care and include: excellence in personnel and staffing; equipment, protocols, and policies; simulation and team training; obstetric emergency management; cesarean delivery and labor analgesia care; recommendations and guidelines implementation; and quality assurance and patient follow-up systems.
We are also very excited to announce that the ACGME has accredited our Stony Brook Obstetric Anesthesiology Fellowship program. This 12-month program provides a comprehensive curriculum for training the next generation of leaders in Obstetric Anesthesiology. The mission of the Obstetric Anesthesiology Fellowship Program is to cultivate Obstetric Anesthesiologists that are passionate about providing safe, high-quality care to all of our pregnant patients. They also will serve as advocates for parturients in order to improve maternal health outcomes.
Division Members
 Assistant Professor Chief of Women's Anesthesia Division |
 Assistant Professor Program Director: Stony Brook OB Anesthesiology Fellowship |
|
 Associate Professor Director of Communication Deputy Chief Medical Information Officer, Stony Brook Medicine |
 Assistant Professor Associate Program Director: Stony Brook OB Anesthesiology Fellowship Director of Resident Education for Obstetric Anesthesia |
|
 Assistant Professor |
 Assistant Professor |
|
 Assistant Professor |
 Professor Ambassador for Diversity |
|
 Professor Vice Chair for Education Director: Residency Training Program Director: Medical Student Education |
Residency Training
We provide the gold standard for obstetric anesthesia care at Stony Brook with two attendings and two residents during the weekdays and a dedicated attending and resident on nights and weekends. We have dedicated daily didactic lectures, and we make a big effort to nurture all of our residents and value their outside lives as well as their work lives. Our diverse patient population on labor and delivery provides a unique environment for our anesthesia residents to work on a multidisciplinary team and improve upon their leadership skills during their rotation. It is fair to say that our resident call room is one of the nicest in the hospital and has become a default resident hangout. It is quite common on any given day to have people wander in and out to eat their breakfast and lunch with us in their L&D home.
We look forward to working with you and teaching you to provide exceptional care of our patients!
We look forward to working with you and teaching you to provide exceptional care of our patients!
Recent Division Activity


Recent Publications
Resident authors denoted by bold type
2025
- Abola RE. My Patient is Twitching Like a Fish Out of Water: Avoiding the Risks of Residual Paralysis. In: Perioperative Medicine: A Problem-Based Learning Approach 2025, Eds: Richman DC, Pulley DD, Oprea AD. Oxford University Press
- Bennici L, Factor M, Singh SM, Costa A. Minimally Invasive Surgery and Other Elements of Enhanced Recovery Protocols. In: Perioperative Medicine: A Problem-Based Learning Approach 2025, Eds: Richman DC, Pulley DD, Oprea AD. Oxford University Press
2024
- Landman UN, Naeem Z, Chen IL, Naeem A, Jaber R. Implementation and mixed-methods evaluation of "Walk with a Doc" program at Stony Brook. J Osteopath Med. 2024 Feb 5.
- Parikh S, Scorsese G, Romeiser J, Bennett-Guerrero E, Costa A, Factor M. Pyxis Proximity Improves Narcotic Waste Compliance Among Anesthesia Personnel. Cureus. 2024 Aug 13;16(8).
2023
- Bargnes V, Corrado T, Abola R. What’s Your No Phone Zone? Sterile Cockpit and Airline Industry Perspectives in Anesthesia Workflow. ASA Monitor. 2023 Aug;87:24–26.
2022
- Qureshi F, Romeiser JL, Murphy PF, Go R, Abola R. A Quality Assurance Initiative on Improving Cefazolin Peri-operative Redose Compliance. Int J Qual Health Care. 2022 Sep 14.
2021
- Winebrenner H, Gelfand H, Roman-Banegas L, Angelo T, Jabaut JM. A Case Report of the Anesthetic Management of a Parturient With Congenital Hypofibrinogenemia and Complete Placenta Previa. A A Pract. 2021 Mar 24;15(3):e01426.
- Costa A, Chandran L, Schabel J, Abola RE, Adsumelli R, Fischel JE. Practice habits in anesthesiology resident education: The impact of feedback using data analytics. Perioperative Care and Operating Room Management 2021 24:100176.
- Abola RE, Schwartz J, Forrester JD, Gan TJ. A Practical Guide for Anesthesia Providers on the Management of COVID-19 Patients in the Acute Care Hospital. Anesth Analg. 2021 Mar 1;132(3):594-604 epub Oct 2020.
- Beg T, Daoud BE, Richman DC. Preoperative optimization of patients undergoing interventional procedures: infrastructure, logistics, and evidence-based medicine. Curr Opin Anaesthesiol. 2021 Aug 1;34(4):482-489.
- Abola RE, Schwartz J, Beg T, Gan TJ, Forrester J. In Response (A Practical Guide for Anesthesia Providers on the Management of COVID-19 Patients in the Acute Care Hospital). Anesth Analg. 2021 Aug 1;133(2).
- Mock S, Jabaut J, Barra D, Angelo T, Benjamin J. Challenges in Obstetric Anesthesia in a Parturient With Native American Myopathy: A Case Report. A A Pract. 2021 Dec 10;15(12):e01541.
2020
- McInerney HJ, Lee M, Saunders T, Schabel J, Adsumelli RSN. Symptomatic Intrathecal Hematoma following an Epidural Blood Patch for an Obstetric Patient with Postdural Puncture Headache: A Case Report and Synthesis of the Literature. Case Rep Anesthesiol. 2020 Mar 18;.
- Landau R, Romanelli E, Daoud B, Shatil B, Zheng X, Corradini B, Aubey J, Wu C, Ha C, Guglielminotti J. Effect of a stepwise opioid-sparing analgesic protocol on in-hospital oxycodone use and discharge prescription after cesarean delivery. Reg Anesth Pain Med. 2020 Nov 10.
Recent Presentations
Resident authors denoted by bold type
2024
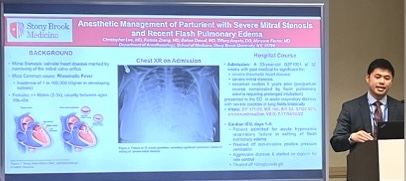
- Lee C, Zhang K, Daoud B, Angelo T, Factor M. Anesthetic Management of Parturient with Severe Mitral Stenosis and Recent Flash Pulmonary Edema. SOAP Annual Meeting 2024
- Aravera C, Angelo T, Daoud B, Factor M. Parturient with Klippel Trenaunay syndrome. SOAP Annual Meeting 2024
- Factor M, Daoud B, Christophides A, Khan A, Stanley S, Bennett-Guerrero E, Angelo T. The Relationship between the High Frequency Heart Rate Variability Index (HFVI) and Epidural Analgesia in the Laboring Parturient. ASA 2024
- Khan A, Angelo T, Stanley S, Factor M, Daoud B. Perception of Preoperative pain as a predictor of Intraoperative Pain During Elective Cesarean Section. ASA 2024
- Angelo T, Daoud B, Factor M, Khan A, Landman U, Garry D, Kimura R, Stanley SL, Bennett-Guerrero E. Randomized Double-Blinded Clinical Trial of Oxytocin Bolus versus Infusion in Elective Cesarean: INBOX trial. ASA 2024
- Singh H, Daoud B, Angelo T, Factor M. Anesthetic Management of a Parturient with Ehlers-Danlos Syndrome and Chiari I Malformation. ASA 2024
- Monanian G, Daoud B, Angelo T, Factor M. Management of Congenital Heart Disease and Valvulopathy in a Parturient. ASA 2024
- Hum B, Shibly Y, Factor M, Daoud B, Angelo T. Management of a Parturient with Alpha-Gal Syndrome and Chronic Pericardial Effusion. ASA 2024
- Shibly Y, Hum B, Factor M, Daoud BE, Angelo TE. Management of a Parturient with Severe SLE and its High-Risk Sequelae. ASA 2024
- Monanian G, Lee C, Daoud B, Angelo T, Factor M. Intraoperative Management of Complete Placenta Previa with Placenta Accreta complicated by Suspected Amniotic Fluid Embolism. ASA 2024
- Marzolini L, Angelo T, Daoud B, Factor M. Approach to the Perioperative Management of Alpha-Gal Syndrome in a Parturient. PGA 2024
- Nguyen N, Bargnes V, Daoud B, Angelo T, Factor M. Angular pregnancy, Asthma, and Apfel: A Triple-A in Obstetric Anesthesiology: Anesthetic Management of a Patient with Angular Pregnancy. PGA 2024
- Nguyen N, Ahn J, Angelo T, Daoud B, Factor M. Anesthetic Management of a Parturient with Congenital Long QT Syndrome. PGA 2024
- Monanian G, Factor M, Daoud B, Angelo T. Intraoperative Management of Complete Placenta Previa with Placenta Accreta complicated by Suspected Amniotic Fluid Embolism. PGA 2024
2023
- Bargnes V, Rakhamimova E, Angelo TE, Factor M, Schabel JE, Daoud BE. Peripartum Management of a Patient with May-Hegglin Anomaly. ASA 2023
- Angelo T, Aravera C, Daoud BE, Factor M. Severe Long Term Sequela of COVID-19 requiring ECMO for CD. ASA 2023
- Shibly Y, Ahn J, Factor MG, Angelo TE, Daoud BE. Management of a Parturient with Severe Mitral Stenosis. ASA 2023
- Gombert A, Fardos Y, Daoud B, Factor M, Angelo TE. Obstetric Anesthetic Considerations and Management in a Patient with Pompe Disease. ASA 2023
- Bargnes V, Rismany J, Schabel JE, Factor M. Peripartum Management of a Parturient with Acute Fatty Liver of Pregnancy and Twin Gestation. ASA 2023
- Rupert D, Wang K, Hafeman M, Lai L, Schabel JE. Publication Rates and Time to Publication for American Society of Anesthesiologists: A Retrospective Analysis. ASA 2023 Shibly Y, Hum B, Taneja K, Schabel JE. Identifying Patients At Risk for Anesthesia-Related Complications During Labor and Delivery. ASA 2023
- Aravera C, Angelo TE. The Lasting Effects of COVID on a Parturient Requiring ECMO for Cesarean Delivery. PGA 2023
- Muncan B, Bell J, Daoud B, Elias M, Factor M, Angelo T. Neuraxial Anesthesia in an Obstetric Patient with Transverse Myelitis. PGA 2023
- Garry E, Elias M, Angelo T, Daoud B, Factor M. Anesthetic Considerations for a Parturient with Congenital Long QT Syndrome and an Implantable Cardioverter-defibrillator. PGA 2023
- Elias M, Rakhamimova E, Factor M, Angelo T, Daoud B. Anesthetic Management of a Parturient with a Symptomatic Pericardial Effusion. PGA 2023
- Daoud BE. Maternal Cardiopulmonary Resuscitation. PGA 2023
- Factor MG. Pain Management Strategies For The Opioid Dependent Parturient. PGA 2023
2022
- Emple A, Nguyen M, Abrahams R, Yarmush J, Schabel J, Banks S, Sagsveen M, Reki A, Straker T, Vanderberg L, Goldstein S. Survey of Patient Blood Management Knowledge Among Anesthesiologist. IARS 2022
- Shuaib K, Koh J, Factor M, Angelo TE, Daoud DE. Anesthetic Management of a Parturient with a Syringo-Pleural Shunt. SOAP Annual Meeting 2022
- Nguyen V, Daoud BE, Angelo TE, Factor MG. Anesthetic Management of a Parturient with a Congenital Factor VII Deficiency. SOAP Annual Meeting 2022
- Angelo T, Factor M, Daoud BE, Kimura R, Khan A, Romeiser J, Bennett-Guerrero E. Randomized Double-blind Clinical Trial of Oxytocin Bolus vs Infusion in Elective Cesarean Section - Inbox Study. ASA 2022
- Daksla NC, Angelo TE. Perioperative Management for Cesarean Section in a Patient with Takayasu Arteritis and Mechanical Aortic Valve. ASA 2022
- Jin Z, Shuaib K, Angelo TE. Anesthetic Management of an Alpha-gal Allergy in a Jehovah’s Witness Receiving a Total Abdominal Hysterectomy. ASA 2022
- Lee C, Daoud BE, Angelo TE, Factor M. Management of Unexpected Anaphylaxis in the Parturient. ASA 2022
- Parikh S, Scorsese GF, Mena S, Cervo K, Diamond P, Kozlowski P, Seiter C, Shafai A, Turkiew E, Giordano Factor M. The Effects of Pyxis Location on the Narcotic Waste Process. ASA 2022
- Qureshi F, Zhang X, Abola RE. Implementation of Automated Reporting of Anesthesia Quality Measures-phase 1. ASA 2022
- Sarwari J, Abola R, Costa A. Retrospective Study On C-Sections With General Anesthesia In A Tertiary Hospital. PGA 2022
- Crugnola W, Costa A, Abola R, Al-Bizri E. Institutional Prevalence Of Sugammadex Use In Pediatric Patients. PGA 2022
- Razak A, Greenspan S, Abola R, Kim J, Daoud BE Considerations For A Parturient With An Implanted Sacral Neuromodulation Device. PGA 2022
- Greenspan S, Bindelglass A, Abola R, Factor MG. Neuraxial Anesthetic Considerations for a Parturient With Factor XII Deficiency. PGA 2022
2021
- Mena S, Gruttadauria M, Factor M, DeLemos M. Spinal Anesthesia in Suspected Brugada Syndrome. ASA 2021
- Parikh S, Alam S, Costa A, Angelo T. Anesthesia For Cesarean Section In A Parturient With Alagille Syndrome. ASA 2021
- Jin Z, Daksla N, Schabel JE, Gan TJ. Efficacy Of Nk-1 And 5-ht 3 Antagonist Combination For PONV Prophylaxis, A Systematic Review And Meta-analysis. ASA 2021
- Turkiew E, Alam S, Schabel J. Peripartum Anesthetic Management Of A Patient With Glanzmanns Thrombasthenia. ASA 2021
- Shafai A, Angelo T, Landman U, Giordano M. Anesthetic Management of a Parturient with Segawa Syndrome. PGA 2021
2020
- Barra D, Mock S, Jabaut J, Patel R, Benjamin J, Angelo T. Challenges In Obstetric Anesthesia In A Parturient With Native American Myopathy. ASA 2020
- Banegas LR, Winebrenner H, Jabaut J, Patel R, Angelo T. Peripartum Management Of A Parturient With Congenital Hypofibrinogenemia And A Complete Placenta Previa Experiencing Vaginal Bleeding. ASA 2020
- Tsai M, Feliciano J, Angelo T. Anesthetic Management For Cesarean Delivery In A Pregnant Woman With Previously Ruptured Cerebral Arteriovenous Malformation. ASA 2020
- Qureshi F, Romeiser J, Abola RE. Preventing Surgical Site Infections (SSI), a QA/QI Initiative on Peri-operative Antibiotic Administration Compliance-timing and Re-dosing. ASA 2020
- Kim B, Costa AC, Schabel JE. Changes in Practice for Obstetric Anesthesia in Parturients During the Covid-19 Pandemic. ASA 2020
- Bracero L, Alam S, Wang E, Costa AC, Schabel JE. Subdural Hematoma Requiring Surgical Evacuation Following Dural Puncture Epidural (DPE): a Newly Reported Complication. ASA 2020
- Alam S, Bracero LA, Costa AC, Schabel JE, Bergese SD. Subdural Hematoma Following Dural Puncture Epidural in a Patient with a Chronic Right Parietal Hemangioma. ASA 2020
- Jin Z, Gan S, Schabel J, Gan TJ. Palonosetron-dexamethasone Combination Vs Ondansetron-dexamethasone for PONV Prophylaxis, a Meta-analysis. ASA 2020
- Shuaib K, Angelo T, Poppers J, Factor M. Anesthetic Considerations in a Parturient with Complex Cardiac History and Pulmonary Hypertension. PGA 2020
- Kant I, Lokshina I, Wang E. Post Dural Puncture Headache Prevention With Abdominal Binder And Bowel Regimen. PGA 2020