
| Volume 27 Number 4 | Stony Brook, NY | < April 2017 > |
 |
|
 Ronald S. Litman, DO is our visiting professor for April 2017. Dr. Litman received a BA in Biology from the State University of New York at Buffalo. Coming to Long Island, he obtained his DO at the New York College of Osteopathic Medicine in 1985. Dr. Litman did residency training in Pediatrics at Rainbow Babies and Children's Hospital, Case Western Reserve University, Cleveland, OH and Anesthesiology at Mount Sinai Medical Center in New York City. This was followed by a Pediatric Anesthesia Fellowship at The Children's Hospital of Philadelphia in 1990-91. A life-long learner, Dr. Litman completed an ML degree in Health Care Law at the University of Pennsylvania School of Law this year. After his fellowship, Dr. Litman joined the anesthesiology department at the University of Rochester initially as Senior Instructor but then was promoted to Assistant Professor and then Associate Professor. While at U Rochester, he held joint appointments in Pediatrics and Dentistry. In 2001, Dr. Litman became Associate Professor of Anesthesiology and Critical Care at the Hospital of the University of Pennsylvania and the Children's Hospital of Philadelphia. Since 2008, he has been Professor at these institutions. Dr. Litman has been very active in several professional societies including the Society of Ambulatory Anesthesia and the American Society of Anesthesiologists. He has been on the Board of Directors of the Malignant Hyperthermia Association of the United States since 2013, has been their Vice President for Scientific Development since 2014, and has been the Medical Director for the MH Hotline since 2013. He has been an Associate Editor for Anesthesiology since 2011. Dr. Litman is prolific! He has authored more than 70 publications in peer-reviewed journals, nearly 60 abstracts for scientific meetings, 124 editorials, reviews and chapters, and has edited four books. We are pleased to welcome Dr. Ronald Litman to Stony Brook Anesthesiology to present two lectures. On Tuesday, April 11, he will speak to the Residents on "My Favorite Malpractice Cases: What I've Learned as an Expert Witness". On the following day, he will present at Grand Rounds: "The Future of Medication Safety in the OR". 
|
 The 2017 Peter Glass Academic Research Evening will take place on Thursday, May 11, 2017. I'll be writing more about the event, including our Keynote Speaker Dr. Mark F. Newman, in next month's issue of SleepTalker. But now is the time to submit your abstracts if you plan to make a presentation! Abstract submission is open to all Residents, Students, CRNAs, Post-docs and Faculty. A select number of abstracts will be accepted for oral presentations. All types of research are welcome: Original Research, Case Reports, and Clinical Concepts and Commentaries. The format for abstracts can be found on the Research Evening web page. Please submit your abstracts to Ms. Christine Fogarty by the April 8, 2017, 5:00 pm deadline. 
|

Christopher Page, MD
Stony Brook Medicine is the first academic hospital in the country to add the IONSYS® fentanyl iontophoretic transdermal system to its formulary. IONSYS® is a self-contained patch that functions as a patient controlled analgesia system. The main advantages of IONSYS® as opposed to traditional IV-PCA appear to be improved patient function and mobility with use of the device. In addition, in existing studies, both patient and nursing satisfaction with the device far exceeds that found with IV-PCA. We will start using this device in the following patients:

|
|
Ralph Epstein, DDS
As I wrote in the January 2017 issue of SleepTalker, the Board of Regents of the NYS Education Department approved updated anesthesia regulations. You can download them here. These regulations go into effect in two phases. Phase one begins in July 2017. It concerns new Definitions (section a) and new Practice Guidelines (section d). Phase two begins in January 2018. This concerns new certification requirements (section b) and new education requirements (section c). Because I was very involved with the development of these updated regulations, I can answer many of the questions you may have. Please feel free to contact me by phone (631-624-7005) or email . 
|
|
Melissa Day, MS, CRNA, CCRN
The Department of Anesthesiology has a dedicated group of Anesthesia Techs who are a vital part of the Anesthesia Team. The Anesthesia Techs assist Providers in setting up the rooms, available to help with patients, turnover of rooms and obtaining equipment and supplies on a moment's notice which allow our Providers to provide quality patient care. We want to Thank our Anesthesia Techs for their hard work, dedication and assistance to Providers. 
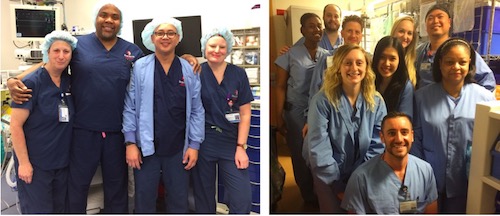
Enjoy more photos from the luncheon on March 31. 
|

|
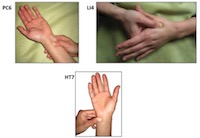
James P. Dilger, PhD

|
|
SleepTalker, the Stony Brook Anesthesiology Newsletter is published by the Department of Anesthesiology
Stony Brook Medicine, Stony Brook, NY Tong Joo Gan, M.D., Chairman Editorial Board: James P. Dilger, Ph.D.; Stephen A. Vitkun, M.D., M.B.A., Ph.D.; Marisa Barone-Citrano, M.A.; Shivam Shodhan, M.D. |











 Deborah Richman, MB, ChB, FFA(SA)
Deborah Richman, MB, ChB, FFA(SA)

