
| Volume 26 Number 4 | Stony Brook, NY | < October 2016 > |
 |
|
|
Stephen Vitkun, MD, MBA, PhD
  The Annual Stony Brook Anesthesiology Alumni Reception!
The Annual Stony Brook Anesthesiology Alumni Reception! Saturday December 10th 2016 (PGA Saturday) from 5 to 7pm Venue: The Yale Club, NYC All Stony Brook Anesthesiology Faculty, Residents and Alumni are invited to attend. Please spread the word to the alumni you know! RSVP to Ms. Martha O'Brien by email or phone 631-444-2904 by November 28. 
|
|
Jun Lin, MD, PhD, has been invited to serve on the ASA Educational Track Subcommittee on Ambulatory Anesthesia for the 2017 Governance Year.

|
 After just over one year, Dr. Aysha Hasan is leaving Stony Brook. She will assume a position at the Boston Children's Hospital. Best wishes! Dr. Hasan has this to say about her stay in our department:
After just over one year, Dr. Aysha Hasan is leaving Stony Brook. She will assume a position at the Boston Children's Hospital. Best wishes! Dr. Hasan has this to say about her stay in our department: "I want to thank everyone for being kind and accepting me as a part of the faculty during this time last year. I had a very nice experience working amongst everyone. I will miss aspects of each and everyone in the department from fellow colleagues, residents, nurses, techs, administrators, and leadership. I have learned a great deal from my time being at Stony Brook and I hope to take some of these lessons to my next journey. I know I will see many if not all of you again later on down the path of my career at conferences and other anesthesia related events. I hope to stay in touch with many of you. My hope, from my time here at Stony Brook, is that I was able to contribute some of my own experiences and knowledge to the department and division to help towards its advancement and progression. Once again, thank you for being a wonderful group of people to be in a practice with. I hope to cross paths with all of you again in the future." 
 Dr. Abdel-Aziz Gaber is retiring. Dr. Gaber studied medicine at Alexandria University in Egypt and did a Surgery Residency at Alexandria University Hospital. After coming to the US, he did a Anesthesiology Residency at MetroHealth Medical Center in Cleveland, OH. This was followed by a Surgery Residency at Robinson Memorial Hospital in Ravenna, OH. In 1999, he came to Stony Brook as an Anesthesiology resident. Dr. Gaber has been an Attending at Stony Brook since 2003. We wish him all the best in his retirement! More photos from recent farewell luncheons. 
|

Department members will be making 36 presentations and moderate an abstract session at the annual meeting of the American Society of Anesthesiologists. The meeting will be held in Chicago from October 22-26. A meeting itinerary can be viewed and downloaded at the Department of Anesthesiology website. (It is on the Quick Links menu found on every webpage).
Please visit our Presenters while you are at the ASA meeting. And, don't forget to take photos of department members standing in front of posters! We can use these in November's issue of SleepTalker, on our website and in the library display case. Medically Challenging Cases
• Abrahams E, Izrailtyan I. Anesthetic Management of a Patient With Subaortic Valvular Stenosis
Oral Presentation
• Abrahams E, Izrailtyan I. Anesthetic Management of Intraoperative Left Ventricular Rupture and Associated Mitral Valve Regurgitation During a TAVR Requiring Conversion to Open AVR • Abrahams E, Schabel JE. Anesthetic Management of an Obstetric Patient With Platelet Storage Pool Deficiency • Abrahams E, Scott B. Pulmonary Hemorrhage after Cryoballoon Ablation for Treatment of Atrial Fibrillation • Fisch AMl, Adsumelli RS. Paradoxical Vocal Cord Motion Disorder: A Typical Cause of Postoperative Stridor Presents a Diagnostic Dilemma for Anesthesiologists • Fischl AM, Loh SA, Bilfinger TV, Izrailtyan I. Removal of an Unstable IVC Thrombus Refractory to Medical Treatment in a Patient With Heparin Resistance • Fradlis A, Kogan A. Caesarean Section in a Patient With Intracranial Schwannoma With Hydrocephalus • Hua B, Adsumelli RS, DeMarco A, Park J. Cerebral Autosomal Dominant Arteriopathy With Subcortical Infarcts and Leukoencephalopathy (Cadasil): Postoperative Care Complicated by Unexpected Pseudoseizures • Hua B, Oleszak SP. Positive Pressure Facilitating Difficult Nasal Intubation • Hua B, Oleszak SP. Tracheostomy Exchange to Tracheal Button for Congenital Hypoventilation Syndrome • Josma J, Schabel JE, Shah S. Wolff-Parkinson-White Syndrome During Pregnancy • Josma J, Steinberg ES, Costa AC, Schabel JE. Management of a Parturient With Brugada Syndrome • Kagan M, Levin S, Epstein RH. Management of a Pediatric Patient Found to Have a Tracheal Web During Endotracheal Intubation • Kagan M, Moon R, Tan M. Mental Nerve Block for Right V3 Postherpetic Neuralgia • Kagan M, Parikh P, Izrailtyan I. The Anesthetic Management of a Patient Having a Balloon Valvuloplasty for Severe Mitral Stenosis With Intraoperative Event of a Third Degree AV Block • Khmara K, Abola RE, Delemos M. Anesthetic Management of Obstetric Patient With Intracranial Cavernous Malformations, Factor VII Deficiency, and Severe Mitral Regurgitation • Kim E. Anaphylactic Reaction During Elective AAA Repair • Moy J, Oleszak SP. Bronchial Blocker for One Lung Ventilation in Resection of Potentially Infected RML • Nelsen D, Praslick A, Panesar R, Seidman P. Utilizing TCOM to Assess Pending Respiratory Failure in PICU • Nelsen D, Stanley SM, Stuart W, Cho B, Schabel J. Psychogenic Seizures after Epidural Local Anesthetic Administration • Nelsen DA, Alcala C, Schabel JE. Anesthetic Considerations for Cesarean Section in Parturient With Cerebral Cavernoma • Nunziata RL, Wang M, Page CR. Emergent Intubation of a Morbidly Obese Patient With Distal Tracheal Mass • Pollack J, Probst S. Anesthetic and Post Operative Management of Venous Air Embolism in the Seated Position • Shodhan S, Gupta R. Airway Management in a Patient With Sturge-Weber Syndrome • Shodhan S, Gupta R. Myoclonic Activity With Low Dose Dilaudid PCA
• Gan TJ, Soergel D, Skobieranda F, Burt D, Cheng J. Duration of PCA Interruptions With Oliceridine (TRV130), A Novel µ-GPS, Versus Morphine
Posters
• Habib AS, Hwang S, Zgheib R, Dhakal I, Greenup R, Gan TJ. Risk Factors Associated With Persistent Pain After Breast Surgery
Panels
• Gan TJ. Novel Anesthetic Drugs in Ambulatory Surgical Practice
Workshops
• Gan TJ. Enhanced Recovery After Surgery in the United States: Implementation and Results in the Perioperative Medicine Era • Grecu L. Updates on the Respiratory Care Management of Patients With Severe Respiratory Distress/Failure
• Stellaccio FS. Difficult Airway Workshop with Simulation
Refresher Course
• Stellaccio FS. Basic and Advanced Flexible Fiberoptic Intubation Workshop
• Gan TJ. Enhanced Recovery Principles for the Ambulatory Patients
Clinical Forum
• Willoughby P. Disaster in the Office (moderator)
Point-Counterpoint
• Willoughby P. Peripheral Nerve Catheters for Outpatient Surgery. Single Shot Blocks.
Scientific and Educational Exhibit
• Gallagher C et al. A Simple Nasal TSE-PAP Mask/Circuit Assembly to Provide Continuous Active Oxygenation During Routine and Emergency Endotracheal Intubation in the OR and at the Remote Locations

|
|
Shivam Shodhan, MD and Ursula Landman, DO

Dr. Rey Llenes presented a study on risk factors associated with ischemic optic neuropathy (ION) by the Postoperative Visual Loss Study Group. He shared how ION can commonly cause visual loss after spinal fusion surgery. The study compared 80 patients with ION to 315 matched control subjects. The various ION-dependent risk factors were male sex, obesity, wilson frame, long surgery duration, larger blood loss and lower percent colloid given. The authors concluded that preventative strategies are the only option to reduce the incidence of visual loss. The ASA practice advisory for perioperative vision loss additionally recommends to use maneuvers to keep the head at or higher than the heart to reduce venous congestion in the head. Additionally, the risk of ION may also be decreased by minimizing the prone position and maximizing hemostasis/minimizing EBL, and using of colloid along with crystalloid. Dr. Aylin Gonzales reviewed a paper on perioperative visual loss in spine fusion surgery by Rubin et al. The study used a large, nationwide hospital database to identify trends and risk factors for ION incidence during spinal fusion. They found that perioperatve ION in spinal fusion decreased 2.7-fold between 1998-2012. Additionally, older age, male sex, transfusion history and obesity were factors that increased the risk of ION. A limitation of the study included not enough data to assess the accuracy of coding complication such as ION (over- or under-coding). Additionally, we discussed the importance of informed consent from surgeons and anesthesiologists, since this is a devastating complication that patients should be aware of and understand. Dr. Rany Makaryus began a multi-part statistical review series which will take place over the Journal Club sessions this academic year. To start off the first review sessions, he focused on the meaning of a p-value. The p-value is defined as the probability of obtaining a result equal to or "more extreme" than what was actually observed, when the null hypothesis is true. He reminded us to that this statistical measure is distinct from clinical significance. Be sure to join us on our upcoming Journal Club this month on October 6th at The Curry Club, where we will discuss nitrous oxide induced PONV and GFR as a predictor of outcomes! Refer to the Journal Club web page for about the papers discussed at this and past Journal Clubs. 
|

TJ Gan is featured on the cover of Anesthesia and Analgesia

|
Shivam Shodhan, MD
|


|
|
Shivam Shodhan, MD
As we awaken to misty mornings and smooth winds rustling the repainted leaves from their trees, it means autumn is here and summer is finally over. Along with the change in foliage comes many treats for everyone. Football season starts, TV shows resume, pumpkin-flavored beers arise, and let’s not forget the return of seasonal coffee flavors (pumpkin spice lattes)! Yes, anesthesiologists love their coffee!
So let’s pack away the trauma season for another few months, grab a nice cup of coffee, take a moment to sit outside on a bench and enjoy the beauty of change. 
P.S. In recognition of the importance of coffee, Stony Brook University just debuted their Starbucks coffee-truck (picture)! It's one of only eight in the country and the first ever in New York State. It will serve the full line of hot and cold beverages, along with pastries, breakfast sandwiches and lunch items, and will be located near the Student Activities Center on the university campus. 
|
|
SleepTalker, the Stony Brook Anesthesiology Newsletter is published by the Department of Anesthesiology
Stony Brook Medicine, Stony Brook, NY Tong Joo Gan, M.D., Chairman Editorial Board: James P. Dilger, Ph.D.; Stephen A. Vitkun, M.D., M.B.A., Ph.D.; Marisa Barone-Citrano, M.A.; Shivam Shodhan, M.D. |




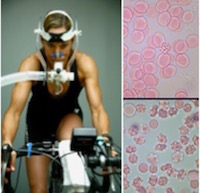 Elliott Bennett-Guerrero, MD has been awarded a grant from the National Heart, Lung and Blood Institute for his proposal "VO2 Max: In Vivo Model for Functional Red Cell Testing. Can RECESS be explained?" Although the FDA permits patients to be transfused with blood that has been stored up to 42-days, the effectiveness of this blood has never been determined.
In his cross-over study, Dr. Bennett-Guerrero will randomize thirty fit 18-40 year old healthy volunteers to receive two units of their own autologous RBCs that have been stored for either 7, 28, or 42 days. He will test the hypothesis that exercise performance (VO2 Max= maximum oxygen consumption) deteriorates after transfusion with RBCs stored for 42 but not 28 days. This is important because no studies have definitively shown that storage duration can affect RBC function. This model holds promise as a rigorous and quantitative in vivo functional assay of RBC function, which can address the quality of the oldest RBCs since a clinical trial is likely not feasible and also addresses an unmet need for future RBC transfusion research.
Elliott Bennett-Guerrero, MD has been awarded a grant from the National Heart, Lung and Blood Institute for his proposal "VO2 Max: In Vivo Model for Functional Red Cell Testing. Can RECESS be explained?" Although the FDA permits patients to be transfused with blood that has been stored up to 42-days, the effectiveness of this blood has never been determined.
In his cross-over study, Dr. Bennett-Guerrero will randomize thirty fit 18-40 year old healthy volunteers to receive two units of their own autologous RBCs that have been stored for either 7, 28, or 42 days. He will test the hypothesis that exercise performance (VO2 Max= maximum oxygen consumption) deteriorates after transfusion with RBCs stored for 42 but not 28 days. This is important because no studies have definitively shown that storage duration can affect RBC function. This model holds promise as a rigorous and quantitative in vivo functional assay of RBC function, which can address the quality of the oldest RBCs since a clinical trial is likely not feasible and also addresses an unmet need for future RBC transfusion research.



