
| Volume 28 Number 4 | Stony Brook, NY | < October 2017 > |
 |
|
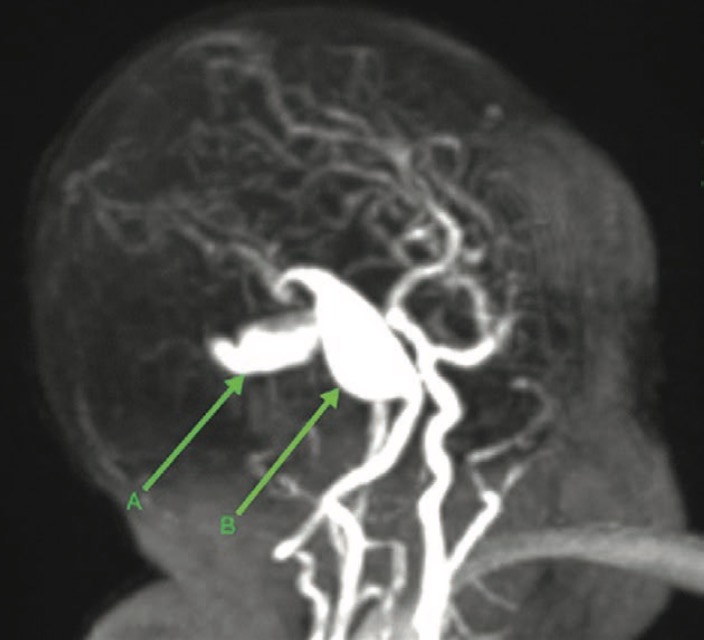
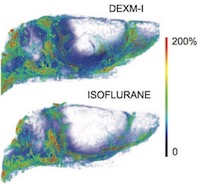
CA-3 Resident Dr. Justin Smith and graduated resident Dr. Scott Licata were coauthors with Dr. Vahe Tateosian on an "Images in Anesthesiology" contribution that will appear in an upcoming issue of Anesthesiology. The image shows two rapidly expanding intracranial arterial aneurysms of the left posterior cerebral artery (A) and left internal carotid artery (B) in a 4.7-kg, 2-month-old, full-term female with SCALP (sebaceous nevus syndrome, CNS malformations, aplasia cutis congenita, limbal dermoid, and pigmented nevus) syndrome. CA-1 Resident Dr. Ehab Al Bizri is a co-author with Attendings Drs. Rany Makaryus and Stephen Probst and Adjunct Faculty member Dr. Helene Benveniste on a paper to be published in Anesthesiology. The paper concerns the effects of dexmedetomidine and isoflurane on solute transport via the glymphatic pathway. See image under New Publications below. Congratulations to CA-1 Resident Leif Ericksen for being the lead author of the monograph “Enhanced Surgical Recovery: From Principles to Standard of Care.” The article is featured in the latest publication of Congress Review, a supplement to Anesthesiology News. It is a review of the Annual Congress of Enhanced Recovery and Perioperative Medicine held on April 27-29, 2017 in Washington, DC. 
|

Department members will be making presentations and moderating sessions at the annual meeting of the American Society of Anesthesiologists. The meeting will be held in Boston from October 21-25.
Please visit our Presenters while you are at the ASA meeting. And, don't forget to take photos of department members standing in front of posters! We can use these in November's issue of SleepTalker, on our website and in the library display case. Medically Challenging Cases
• Adrahtas D, Azim S. Multi-trauma patient with deteriorating mental status in PACU: Isolated Cerebral Fat Embolism
Posters
• Escobar D, Scott BH. Unilateral Tympanic Membrane Rupture During Robotic-Assisted Laparoscopic Prostatectomy • Georges R, Schabel J, Wang M. Convulsive Syncope vs Eclampsia • Licata S, Tateosian V. Difficult Airway Management in a 21 Month Old with Cornelia de Lange Syndrome • Na Javeed S, Azim S. Cardiac Arrest after Tourniquet Release for Knee Arthroplasty or Anaphylaxis • Ni S, Hua B, Schabel J. Ephedrine-Induced Myoclonus in a Parturient • Smith J, Licata S, Tateosian V. Management of Two Large Intracranial Aneurysms in a 2-Month-Old Female • Thalappillil R, Azim S. Awake fiberoptic intubation in a morbidly obese male with large right submandibular and sublingual abscesses: a comprehensive, multimodal approach • Thalappillil R, Scott BH, Seifert FC. Resource utilization, Postoperative mortality and morbidity in octogenarians, our experience 10 years later • Thalappillil R, Izrailtyan I, McLarty HJ. Role of intraoperative TEE in identifying previously unrecognized RA thrombus prior to LVAD placement in patient with decompensated idiopathic dilated cardiomyopathy • Zia H, Oleszak SP, Andraous W. Complex Airway Management for Vocal Cord Lesion, Partial Glossectomy, Partial Palatectomy, Tonsillectomy, Pharyngectomy and Radical Neck Dissection combined
• Liu L, He J, Zhu J, Rebecchi MJ. Age Associated Cardioprotection Differences by GSK3β Inhibitor in Rat Heart: Effects on Autophagy Pathways
Panels
• Viscusi ER, Skobieranda F, Soergel DG, Burt DA, Gan TJ. APOLLO-2: A Randomized, Double-Blind, Placebo- and Active-Controlled Phase 3 Study Investigating Oliceridine (TRV130), a Novel μ Receptor G Protein Pathway Selective (μ-GPS) Modulator, for the Management of Moderate to Severe Acute Pain Following Abdominoplasty • Richman D. Perioperative Medicine Poster Discussions (moderator) • Richman D. Perioperative Medicine Poster Presentations (moderator)
• Gan TJ. Opioids in Acute Pain Management - Friend or Foe: An Evaluation of Safety and Utility
Workshops
• Gan TJ. The Role of Novel Analgesics and Monitors to Assess Pain
• Stellaccio FS. Difficult Airway Workshop With Simulation
Point Counterpoint
• Gan TJ. Neuromonitoring Should Become a Standard of Care in the Ambulatory Setting
Clinical Forum
• Willoughby P. My Patient is Shaking, Stiff and Won't Talk but It's Just Ambulatory Surgery: What Do I Do? (moderator)

|

|
James P. Dilger, PhD

|
Marisa Barone-Citrano, M.A.
|

Jean Abbott, BS, MT 
Darcy and I went to the Docs Who Rock fundraiser, where we listened to our very own Jamie Romeister as lead singer and keyboardist of the group Prognified. Jamie was great! |

Adrian Fischl, MD 

|
|
SleepTalker, the Stony Brook Anesthesiology Newsletter is published by the Department of Anesthesiology
Stony Brook Medicine, Stony Brook, NY Tong Joo Gan, M.D., Chairman Editorial Board: James P. Dilger, Ph.D.; Stephen A. Vitkun, M.D., M.B.A., Ph.D.; Marisa Barone-Citrano, M.A.; Shivam Shodhan, M.D., M.B.A. |














